When we think about antibiotics, we think about how they help us recover from illness, or visits to the GP to get a prescription for ourselves or our children. We think of a medication readily available to help us fight infection.
What we’re unlikely to think about is a world where we don’t have them at our disposal at all.
But this is exactly what I want you to think about. Why? Because our antibiotics that we use every day are under threat due to increasing amounts of bacteria that are resistant to them. This might seem like a problem for doctors and scientists to deal with, but that’s not the case.
So who needs to be worried about this? The answer is all of us. It doesn’t matter if you or your family rarely need antibiotics - if we lose these medicines everyone loses out.
Yes, antibiotics are used for common infections, such as pneumonia and kidney infections, and we rely on them to treat these, but they’re needed for much more too. They treat infections after lifesaving transplants and other surgeries, childbirth, cancer treatment, the list goes on. They save lives, they treat our loved ones and they are an essential part of modern medicine. One in three of us takes at least one antibiotic each year.
One reason antibiotic resistance has happened is through inappropriate use and over-prescribing. We take them for illnesses they can’t treat, we don’t take them properly or we ask for them when we don’t need them. All of this puts our future healthcare at huge risk.
An example of inappropriate use is taking them when we have coughs, colds and flu. We know that more than half of those who attend the GP with these symptoms get prescribed an antibiotic, and this has increased over the last 10 years. But antibiotics do not treat viruses, such as colds or flu.
Yes, you may feel awful when you have a virus, but taking an antibiotic won’t change that, it will just alter the bacteria in your body, kill healthy bacteria and allow the bacteria that are resistant to the antibiotics you have just taken to become dominant. This means that when you DO need an antibiotic, it is less likely to work.
Bacteria live in all of us and outnumber our human cells tenfold, and the majority of these bacteria are essential. They help us digest food, produce important vitamins and keep up our immunity. It’s vital to our wellbeing that we have these good bacteria, but each time we take antibiotics, we kill many of them.
It can take a long time - from months up to years - for the good bacteria to recover, so we must be careful. If we don’t absolutely need to use antibiotics, we really shouldn’t take them.
Urinary tract infections (UTIs) for example are extremely common and require antibiotics, but in Europe bacteria causing UTIs are already commonly resistant to many of the antibiotics used to treat them.
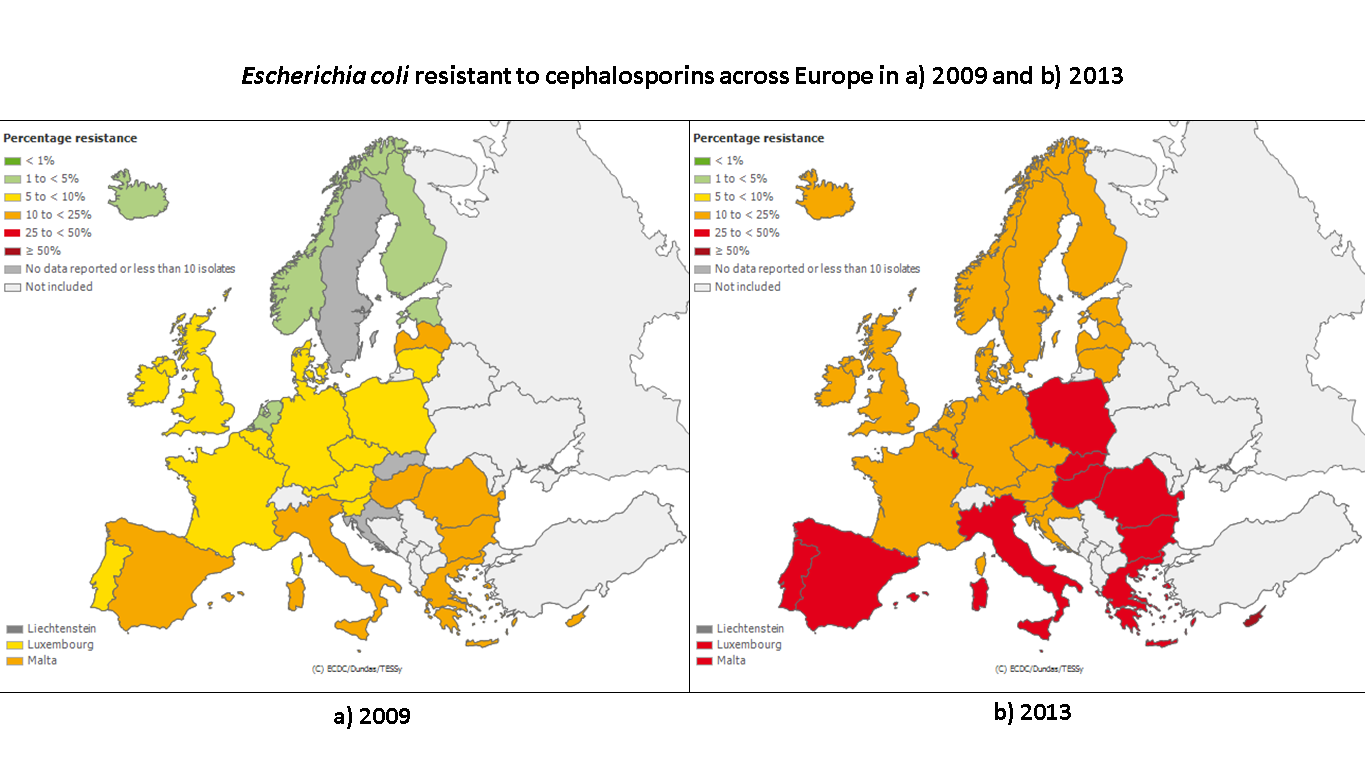
This spread of resistant bacteria is happening quickly. You can see below for example, that in just 5 years, antibiotic resistance in the commonest bacteria causing sepsis in Europe has increased dramatically. If we continue with this trend, in 10 years Europe could be in serious trouble with infections that have few or no antibiotics that can be used for treatment.
The most straightforward solution would be discovering new antibiotics, but of course it isn’t that simple. Penicillin was discovered in 1940, some 75 years ago, and since then discoveries have declined. It’s been 30 years since a new major antibiotic was discovered, which means we must preserve what we have.
So what can we do to fight back against resistant bacteria? Firstly, it’s important we stop asking for and taking antibiotics every time we feel ill.
Equally, it’s important our doctors stop prescribing them for problems they can’t treat, so if your GP doesn’t offer them you shouldn’t put pressure on for a prescription. If they do offer them why not ask whether there are alternatives that you could use instead, or whether you could get a back-up prescription to take if you feel worse in the next few days?
And when taking children to see a doctor, though it’s understandable to want a prescription to help them feel better, antibiotics will rarely be the answer. Protect the good bacteria in your children’s gut, as doing so will keep your children healthy and help their immune systems work effectively!
To tackle this issue we need to treat ourselves and our own health better, which incidentally is what self-care week is all about. Starting 16th November, the week will highlight the importance of choosing the right local health services so that everyone can get the best out of the NHS. Reducing our use of antibiotics for conditions that we could actually treat with medicines available without prescription is part of this.
We also need to do more to reduce the risk of infection in the first place, and not just bacterial infections. We should make sure that our children, older people and other vulnerable people are vaccinated against flu. This year the flu vaccine will be offered to all children aged two, three and four and in school years one and two. If you or your child is in one of the groups recommended for vaccination, we urge you to take this opportunity.
Women can also take some simple steps to reduce the risk of cystitis and kidney infections (urinary tract infections) including drinking lots of water, taking showers rather than baths, educating themselves on appropriate personal hygiene, wearing clothing that can help reduce infection from gut bacteria and urinating after sex.
Protecting the antibiotics we have requires action. It’s a scary thought to think about a post-antibiotic era, but acting now can prevent this becoming reality.
Please sign up and support the fight to save our antibiotics by choosing a simple pledge at www.antibioticguardian.com. Please share the campaign and spread the word.
Image: rltherichman