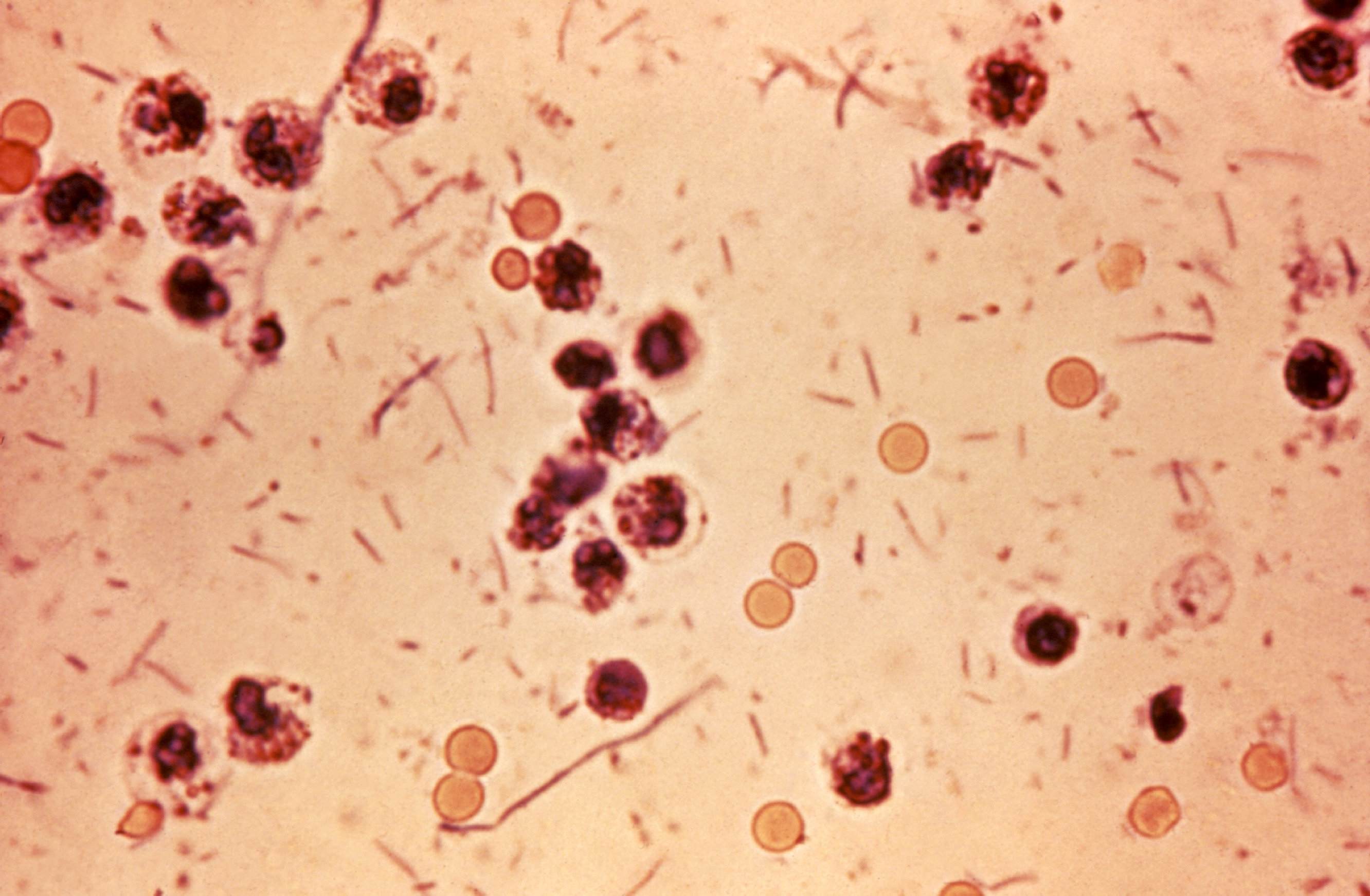
It’s worrying to see new figures showing a sustained increase in cases likely to have been sexually-acquired between men who have sex with men (MSM).
Historically Shigella infections in adults in the UK were mainly due to overseas travel. However, in recent years there has been a large increase in diagnoses of Shigella among men whose infection was not associated with travel, while diagnoses in women remain stable.
In England, there were nearly five times as many adult male cases of Shigella without a known travel history than female cases in 2015. This represents an excess of 500 male cases compared to females, which is more than three times more than reported in 2011. Affected areas include London, Brighton and Manchester.
What is Shigella?
Shigella is a serious gut infection causing severe, prolonged diarrhoea and stomach cramps.
Among gay and bisexual men it’s thought to be spread primarily through the faecal-oral route during sex, either directly or via unwashed hands and only a tiny amount of bacteria is needed to spread the infection.
People can get Shigella by licking skin, condoms, or toys which have faeces on them, even when this is not visible.
Symptoms often develop around 1-3 days after sex and include frequent and explosive diarrhoea (sometimes containing blood), stomach cramps, feeling feverish and some people even report vomiting.
Men experiencing these symptoms should be advised to visit their doctor or a sexual health clinic to get tested, explaining that they may have picked up a gut infection from sex, possibly Shigella. The infection is treatable.
Raising awareness
To reduce the increasing rates of Shigella in England, we need to raise awareness of the risks, and crucially, how people can lower their risk of infection.
To lower the risk gay and bisexual men are advised to:
- wash their hands after sex (and buttocks and penis too if they can, by showering), especially if they’re fingering or handling used condoms, wash sex toys or douching equipment.
- change condoms between anal and oral sex
- use a barrier for rimming (such as a square of latex)
- use latex gloves for fingering or fisting
We’ve distributed posters and leaflets to sexual health clinics, highlighting the symptoms of Shigella, how it is transmitted and how to avoid it. These resources can also be downloaded for use here.
MSM with Shigella may present to a range of healthcare settings and often not to specialist sexual health clinics. In the event of a Shigella diagnosis in a man, particularly where this is not associated with travel to an endemic area, a sexual history should be sensitively obtained.
Patients reporting same sex partners are likely to be at risk of other sexually transmitted infections and HIV co-infection so clinicians should consider referral to sexual health services for appropriate HIV/STI screening, partner notification and prevention advice.
In addition to advice about handwashing, food handling, personal hygiene, and returning to work, MSM diagnosed with Shigella should be advised about the risk of sexual transmission and to avoid sexual activity for at least one week after symptoms cease.
Professional resources
We provide a number of resources, such as expert data on on-going and emerging outbreaks of sexually transmitted infections, including Shigella.
This information can be useful when looking at the issues within a local community, and tailored activity to address them.
Our ‘Health Protection Reports’ provide regular data updates and commentary on infectious diseases. In July 2016 a report specific to Shigella was published.
Eurosurveillance also published a report on Shigella, which provides advice about STI screening for identified cases of the infection.
For members of the public, those worried about Shigella can find out more by visiting NHS Choices.

