
I was recently invited to an All Party Parliamentary roundtable to explore how we will implement recommendations from the 2016 parliamentary report on behaviour change, information and signposting.
These actions will support the NHS Five Year Forward View commitment to enable population prevention at scale.
The major causes of premature death in the UK – cancer, heart disease, stroke, respiratory disease and liver disease – are all linked to behavioural risk factors such as smoking, drinking too much alcohol, lack of physical activity, poor diet and being overweight.
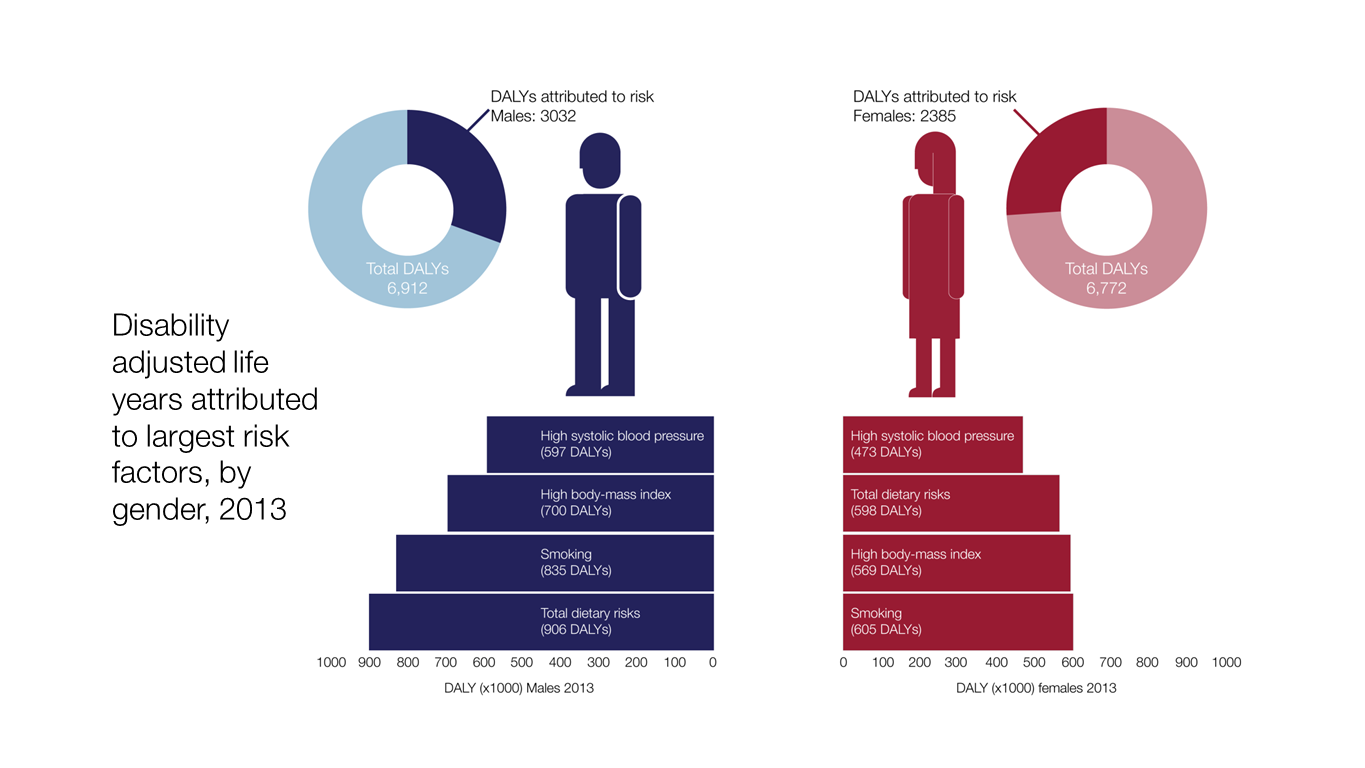
These risk factors are responsible for 40% of disability adjusted life years (years lost due to ill-health, disability or early death) in the UK, yet for many people, they can be modified by a change in lifestyle.
Behavioural change – modifying behaviour to improve health – is fundamental to the prevention agenda to improve health outcomes against a backdrop of rationalisation and squeezed budgets.
Making changes such as stopping smoking, improving diet, increasing physical activity, losing weight and reducing alcohol consumption can help people significantly reduce their risk of disease and help to achieve long-term health, social care and public sector savings.
We're working to support population behaviour change in a number of ways, and developing new tools to maximise the contribution and impact of our behaviour change interventions.
Public-facing campaigns
Our public behaviour change campaigns tackle some of the most serious health issues faced by society, from sugar consumption and drinking too much alcohol to being able to identify the symptoms of cancer.
Change4Life is our flagship programme for preventing childhood obesity, and supports people to eat a healthier diet and be more physically active. The January 2016 Change4Life Sugar Smart campaign inspired more than 2 million downloads of the Sugar Smart mobile app. A survey of 1001 mums who had used the app found 96% of those with 5-11 year old children agreed the app has prompted them to make a healthy change to cutting their families sugar intake.
Earlier this year we launched One You, a campaign to support adults across the country to avoid future diseases caused by modern day lifestyles. It provides a range of tools and advice to help people take action on everyday behaviours such as eating too much unhealthy food or continuing to smoke. More than 1 million people have completed our How Are You quiz, more than 70% of whom have already taken action to better protect their health.
Behavioural insights
PHE’s behavioural insights team applies behavioural science – a range of approaches that seek to understand and modulate human behaviour – to the design, delivery and evaluation of public health practice. The team works with public, private and voluntary organisations to conduct robust testing, including randomised control trials, to help ensure that policies are rigorous, evidence-based and cost-effective.
Recent examples of their work include increasing uptake of lifestyle services by overweight children using a behavioural-informed feedback letter to parents and increasing healthy food choices by NHS staff through tailored promotions, pricing and labelling.
Making every contact count
There are millions of interactions taking place between health professionals, organisations and the general public every day that provide the opportunity to have a conversation to improve health.
Making Every Contact Count (MECC) is an approach to behaviour change that enables the opportunistic delivery of consistent and concise healthy lifestyle information to support people in making positive changes to their physical and mental health and wellbeing.
The focus for a MECC brief intervention might be on individuals losing weight, quitting smoking, reducing alcohol intake, or helping to reduce social isolation. MECC includes short signposting conversations to refer people to more active interventions such as stop smoking services.
Drawing on behaviour change evidence, PHE has worked with Health Education England and NHS England to lead a national MECC advisory group to develop a suite of practical resources to support the uptake of the MECC approach. The NHS Standard Contract also now requires providers to develop and maintain an organisational plan for making every contact count.
Reaching further through pharmacies
PHE supports and provides strategic leadership for the acceleration of the Healthy Living Pharmacies (HLPs) programme. Pharmacies wishing to become HLPs have to satisfy quality criteria and have three enablers in place including a qualified health champion on site; premises that facilitate health promoting interventions with a dedicated health promotion zone; and local stakeholder engagement.
There are now more than 2,100 Healthy Living Pharmacies and over 3,500 qualified health champions who reach out to local communities and engage members of the public to promote health interventions, making every contact count.
We produce dedicated pharmacy campaign toolkits for some campaigns such as Stoptober, Be Clear on Cancer and Stay Well This Winter that can be ordered free of charge to help make supporting our campaigns as simple as possible for pharmacy teams.
Supporting professionals
PHE has provided input to the new national framework for nursing, midwifery and care staff Leading Change Adding Value, which has a focus on helping to prevent avoidable illness, protect health and promote population well-being and resilience.
The NHS engages with over 1 million individuals every 36 hours across the UK, meaning there are many opportunities for health care staff to encourage healthier behaviours during routine consultations and in daily contact with individuals and the community. The NHS Health Check programme is a prime opportunity for healthcare staff to raise lifestyle issues and to suggest behavioural interventions. For instance, many people are now being referred onto the NHS Diabetes Prevention Programme, designed to communicate to patients how their behaviours can help them to reduce their risk of premature ill health and the complications associated with Type 2 Diabetes.
PHE’s work in the Humber also illustrates this approach, where a prevention-based training programme for primary care dental teams has been developed with Health Education England and key partners, which includes a tailored ‘MECC- Level 1’ training resource for primary dental care teams.
All of this work links closely with the PHE-led All Our Health call to action, which provides online resources for healthcare practitioners to help develop their skills working with individuals to prevent illness, protect health and promote wellbeing and self-care, through approaches such as MECC.
Local authorities have enabled a wide range of partners and frontline services to become engaged in behaviour change activity including allied health and social services, fire and rescue teams and housing services.
For example, Staffordshire County Council has worked with the local fire service and the RNIB to provide free eyesight screening tests during the Home Fire Risk Checks service and signpost people to appropriate services. As a result, older people who have engaged with the project now have a better understanding of their eye health and improved levels of confidence and are actively helping others through peer support or campaigning.
Further resources to support PHE led campaigns, such as One You can be found via the Campaign Resource Centre.
Swimming image: Sport England
