Field epidemiology is one of the mainstays of examining outbreaks of infectious disease. Public Health England’s field epidemiology service (FES) contributes to investigating anything from the more common food poisoning incidents to the more exotic such as the new MERS-Coronavirus recently identified in the Middle East.
There are three key areas:
Monitoring and identifying health threats
To be effective we need to be constantly on the lookout for anything unusual so we review our surveillance information regularly looking for any changes that may be of concern. We do this by using data from NHS laboratories and clinics to help us to identify outbreaks of infections such as meningitis, measles or flu. We also undertake surveillance to monitor the health effects from exposures to environmental hazards.
Outbreak and incident investigation
When we identify an outbreak or any other situation that requires prompt public health action we ask ourselves ‘What is the source of this outbreak?’ To answer this question we use scientific answer studies. So for example if this was an outbreak of food poisoning we would contact the people who became ill to find out what they ate and where they went before they became unwell.
From these conversations we may get some clues that help us develop hypotheses that we then test using methods such as case-control studies. This often involves checking what the people who became ill (cases) did compared the people who did not become ill or to a sample of the population (controls).
The other very important question is ‘How can we stop the outbreak?’ We use information from our investigations to put in place measures to control the spread of infection. This could include removing a product from the market, closing a care home to new admissions or offering antibiotics to contacts of cases with an infection such as meningitis.
This element of the FES can be seen in this example where we supported a local investigation into an outbreak of Salmonella Goldcoast. This is an uncommon strain in the UK, and the cause was unknown. We undertook an epidemiological investigation, working with the Food Standards Agency and local authorities, to identify the source and prevent other people from becoming ill.
The findings from the epidemiological study were supported by microbiological and environmental investigations. This included tracing of suspected food items – in this case whelks - from a particular producer which were found to be the source of the outbreak. The product which may have been contaminated was recalled. To our knowledge, this outbreak is the first known report of bacterial food poisoning associated with eating whelks. This information can now be used to prevent outbreaks in the future.
The final question is ‘Are the control measures working?’ Implementing control measures is not enough - we need to check that they are working.
Like so much in life, timing is very important. The quicker the response to an outbreak starts, the more we can reduce both harm to people and the impact on health services. The graph below shows the benefits of early identification and response. A similar ‘real-life’ example would be the international response to the SARS virus back in 2002.
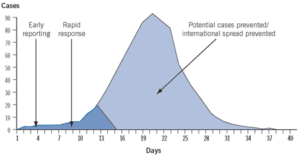
Epidemiological methods are also used to inform policies that are aimed at the control of infectious diseases.
Field epidemiology in action
Field investigations are often complex and we work like detectives to solve mysteries. The following is an example of a investigation that is typical of the sort of issues that we face.
This outbreak of gastrointestinal illness made the BBC News. (See a full report of the Thames outbreak here)
Around 1,100 people took part in the 2 mile open charity swimming race between Hampton Court and Kingston Bridge on the river Thames. Following the race over 300 people reported having been ill with gastrointestinal illness.
Initially the FES were notified of one person who was hospitalised with severe headache, nausea, fever and sweating. Two friends of the patient who participated in the race were also ill.
FES staff and the local health protection team interviewed affected individuals over the weekend. The use of social media helped us in our investigations as around 40 people had reported illness following the event on a Facebook page. We contacted the organisers, a professional sports event company, who assisted us in the investigations.
In this case the event had concluded and the risk was in the past, but it was important to undertake an investigation to help us understand and prevent similar problems in the future. We invited all the race participants to complete an on-line survey with the aim of identifying how many people had been ill, and what factors contributed to their illness.
Of the 1,100 people we surveyed, approximately 60 per cent replied. About half of them had been ill. The river Thames is known to be regularly contaminated with sewage but here is no routine monitoring of water quality as it is not designated as bathing water.
We identified two main things that were linked to being ill: wearing a wetsuit and swallowing water during the swim.
We considered that the link between wearing a wetsuit and illness may have been due to inadequate cleaning and hand hygiene when handling the wetsuits after swimming. The suits would be contaminated when the water is contaminated. If swimmers then ate or drank without washing their hands they could have acquired an infection. Our advice in this instance is that while we are not recommending that people stop wearing wetsuits, we do recommend that they are cleaned thoroughly after use.
This work was important because open water swimming is growing in popularity in the UK and many people may not be aware that swimming in natural rivers and lakes can carry a risk of infection. Following this outbreak we have developed advice and practical tips to assist open swimming event organisers to help people to protect themselves from infections.
Those of us who work in the FES for PHE have a goal to develop a strong network of highly skilled field epidemiologists with a shared sense of purpose, and working to common standards across the UK and Europe. We also want to raise the profile of field epidemiology so that it becomes established into everyday health protection practice and improves links with the broader public health system. To increase the capacity and provision of public health epidemiology services, PHE runs a Field Epidemiology Training Programme to provide state of the art training in field epidemiology enabling its fellows to apply epidemiological methods to a wide range of public health problems in the UK.
If you fancy yourself as a scientific Sherlock, why not take a look at our two year postgraduate training programme aimed at health professionals with a keen interest in applied health protection epidemiology and who wish to develop their specialist field epidemiology skills?
