All newborn babies in England are now being offered screening for four additional rare genetic disorders through the expansion of newborn screening.
The current NHS Newborn Blood Spot Screening Programme now includes screening for: homocystinuria (HCU), maple syrup urine disease (MSUD), glutaric aciduria type 1 (GA1) and isovaleric acidaemia (IVA).
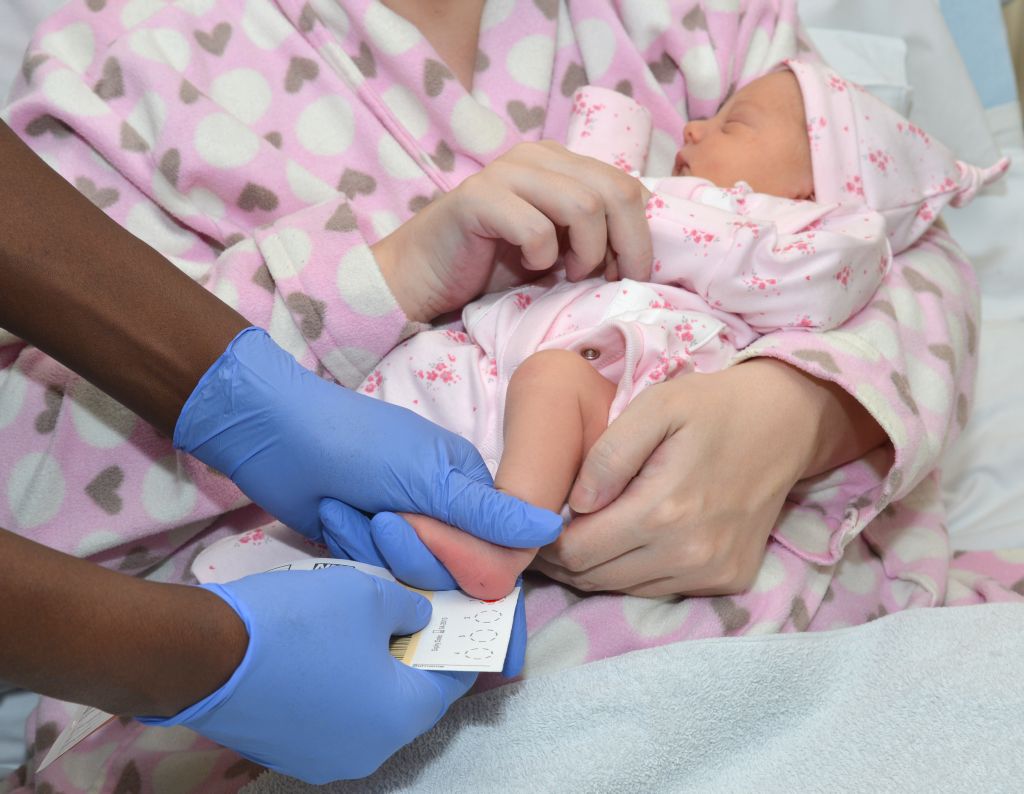
The programme, which involves a heel prick blood test when a baby is five to eight days old, already screened for: phenylketonuria (PKU), congenital hypothyroidism (CHT), sickle cell disease (SCD), cystic fibrosis (CF) and medium-chain acyl-CoA dehydrogenase deficiency (MCADD). Last year more than 1,400 babies, out of 694,000 screened, tested positive for one of these serious conditions.
Testing for these conditions, leading to early detection and treatment, will prevent those babies affected from dying or being severely disabled for the rest of their lives. Therefore it is not surprising that the UK National Screening Committee (UK NSC), which recommends which conditions should be screened for in the UK, is often called on to screen babies for more conditions.
Some may question why we are now screening for more rare conditions and not for other serious conditions that are more common.
Why screen for these particular very rare conditions?
Although the additional four conditions are rare, affecting about 30 children a year in England, the early detection and treatment for those babies affected is life-changing.
In England we have screened babies for the rare conditions phenylketonuria (PKU), and medium-chain acyl-CoA dehydrogenase deficiency (MCADD) for many years. Like PKU and MCADD, the additional disorders are all recessive inherited metabolic diseases and if not picked up early, they almost always cause severe developmental problems, including serious mental disability and possibly coma, or even death.
These conditions require lifelong management through special diets and in some cases, supplementary vitamins or medicines. But early, well managed treatment following early detection means these babies can live normal, healthy lives.
In addition, the tests that are used are proven to be very accurate at finding those babies with the diseases. This was shown through the results of an extensive pilot programme, coordinated by Sheffield Children's NHS Foundation Trust.
The pilot screened over 430,000 babies for these rare conditions and proved the effectiveness of the tests, treatment and suitability for screening, showing the benefits of doing so outweighed the possible harms.
What could be the harm in screening babies for more conditions?
The UK NSC’s recommendation on screening for a condition is based on the evidence against strict internationally respected criteria, at the heart of which is making sure that screening would provide real benefit to the baby and their parents.
These considerations include:
- How good is the test? If the test is not reliable some parents will be unnecessarily worried and may receive worrying advice or unnecessary tests and treatments while others may be falsely reassured and so dismiss important symptoms when there is actually a problem
- Does the test accurately predict who will get the disease and do we know enough about the condition? Especially when that condition may be incredibly rare, we need to be able to accurately tell who will be affected as some may never develop any symptoms
- Do we have an effective treatment? For example, for some conditions where there is no available treatment, knowing your baby has a condition and not being able to do anything about it can be harmful, especially during the special bonding period between parents and baby shortly after birth. The question is; what would be the benefit of knowing this diagnosis at birth when there is nothing that can be done?
Are we likely to see screening for more rare conditions in the future?
Earlier this month the UK NSC recommended against screening for the rare genetic condition, Gaucher disease. This is because it is not currently possible to predict how severely an individual detected through screening might be affected by the condition, meaning some parents may be told their baby has the condition when there may never be any symptoms. In addition, it is unclear whether earlier treatment as a result of screening would bring more health benefits than later diagnosis and treatment following the development of symptoms.
The UK NSC is currently assessing a number of other rare conditions that could potentially be included in the NHS Newborn Blood Spot Screening Programme. As with all screening programmes, these would only be introduced if it is clear that the benefits to newborn babies outweigh any potential harm.

1 comment
Comment by Bren posted on
Hello Anne,
Thanks very much for the blog.
The additional screening will help more of the early detection and therefore early treatment for the babies. In doing so, and as you have cited, the severe development problems in later life.
I can definitely see the need for the UK National Screening Committee so as to ensure proper governance.
The only thought I would add is for the lay explanation of the diseases cited in this blog.
Best wishes and thank you,
Bren.