This week the Mental Health Taskforce published its engagement report, highlighting what 20,000 people think the priorities for the country’s mental health are. The report underlines the importance of mental health nationally and the chance we now have to make a significant change within a generation. Encouragingly, one in four of the responses identified prevention as a key priority for action by 2020 and beyond.
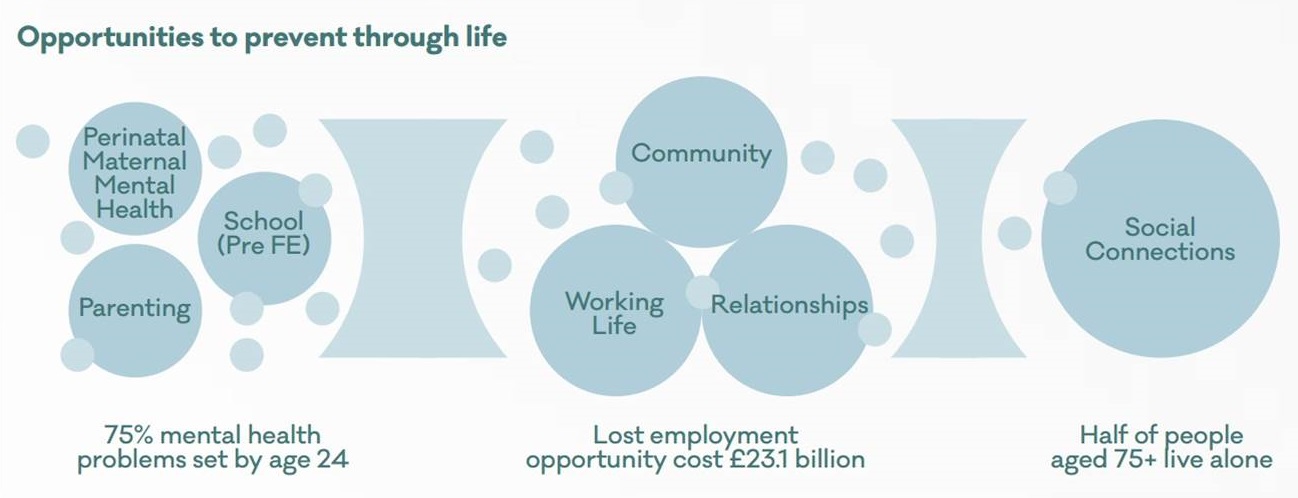
Image: Mental Health Foundation
At PHE we are committed to prevention and to improving the country’s mental health and are working with our partners to help achieve this required shift to prevention. The work of the mental health taskforce is part of the 5 Year Forward View – and the Prevention Board that supports this is chaired by PHE’s chief executive Duncan Selbie.
I am proud to be a member of the Mental Health Taskforce and to be leading PHE’s work on mental health. In our new PHE action plan for 2015/2016, and in our October 2014 Evidence into Action priorities document we highlight the importance of mental health.
Our work so far on mental health includes:
- establishing the ground breaking National Mental Health, Dementia and Neurology Intelligence Network with NHS England
- leading on the public mental health leadership and workforce development framework
- delivering a series of products to improve the lives of those living with and recovering from mental illness - Smoking cessation in secure mental health settings and The Lester Tool
- developing guidance for schools and colleges on children and young people’s emotional health and wellbeing.
In addition, we have issued Guidance for developing a local suicide prevention action plan, launched a Local suicide prevention profile tool and commissioned an innovative, national web-based platform for people with mental health difficulties to share their lived experiences - ‘A day in the life’.
Finally, we have set out our approach to community-centred approaches that improve resilience, health and wellbeing and worked closely with the team from the What Works Centre for Wellbeing, as we look beyond illness into the assets that individuals families and communities can bring to prevent mental illness and promote healthier lives.
Looking ahead, we and our partners are determined to make the prevention of mental illness a key feature of national work. We need to think and act differently if we want to achieve different results and this is a significant opportunity for a step change towards prevention.
This is exactly the reason why we have established the National Prevention Alliance for Mental Health – a group of over thirty organisations with a passion for collaborative working and making a difference.
As an alliance, we are committed to addressing the social determinants of mental health; good jobs, decent homes, supportive friends and family, quality education, accessible healthcare and a living income. We also want to support:
- the development of a national mental health and wellbeing literacy programme
- using intelligence wisely for prevention
- encouraging the adoption of community based approaches to help harness local assets and the potential of strong local social networks
- building the capacity, skills and confidence of the workforce.
We will also continue to focus on and support the implementation of the National Suicide Prevention Strategy, improving the health of people with a mental illness and those with a long term condition (mental and physical long term condition or disability including learning disability) and improving mental health across the life course.
Building our knowledge about what works for prevention also depends on developing a research programme on public mental health and wellbeing.
I am dedicated to championing good mental health in our country and motivated by this biggest chance in a generation to make a real difference.
There is a lot to be done. Over the next few weeks we will be working with our partners to develop a set of practical recommendations that will make a real impact over the next 5 years and I look forward to the publication of the Taskforce’s full report in October.
I am dedicated to championing good mental health in our country and motivated by this biggest chance in a generation to make a real difference. We must and will do more together to put prevention at the heart of mental health.

3 comments
Comment by Mark Gamsu posted on
Thanks for this blog Kevin. I am pleased that prevention has rightly found its way up the agenda .
However, I am disappointed that both Public Health England and NHS England continue to fail to respond to the impact that the wider Social Determinants have on the lives of people with a Psychosis.
There is a good evidence base of the two way relationship between psychosis and issues like problematic debt and housing insecurity. People with a psychosis are 4 times more likely to be in problematic debt than those who are well.
Recent work by the Centre for Mental (http://www.centreformentalhealth.org.uk/welfare-advice-report) highlights the importance of systematic assessment and access to welfare rights advice for this extremely vulnerable group - and the impact this can have on their recovery and helping them to stay well.
Yet, it is the case that very few NHS Care Trusts and CCGs provide or commission a comprehensive welfare rights service for people on the Care Programme Approach. I would like to understand why PHE and NHSE seem reluctant to take any action on this issue. Just to declare an interest I am a Trustee of Sheffield CAB (who are one of the few bureau providing a targeted service to people with a psychosis) and a Trustee of Citizens Advice. @markgamsu
Comment by Gregor Henderson posted on
Your comments and challenges are very welcome. We are in agreement with you on the evidence and the pressing need to develop in partnership with others a more proactive response. The recent excellent Centre for Mental Health report provides us all with a good roadmap. We’d be keen to do more work with partners and I will get in touch with you directly to explore what we can do together.
Currently we’re organising a national conference (http://www.kingsfund.org.uk/events/housing-and-public-health) at The King’s Fund on October 21st 2015 on housing and health. Mental health will be one of the key areas identified as needing national attention and Duncan Selbie will be talking at the conference. Our colleagues in the Mental Health Intelligence Network collect a range of indicators around Serious Mental Illness and the Psychosis Care Pathway, which can be found here (http://fingertips.phe.org.uk/profile-group/mental-health/profile/severe-mental-illness) and include wider social determinants such as socioeconomic deprivation, unemployment and homelessness. Also, the work around community-based approaches Kevin mentioned in the blog is vital for people living with mental illness.
PHE is doing what it can to help coordinate work, share experiences, raise the profile of important issues and help get them attention through our networks and national leadership / coordination role. There is now a key opportunity of linking the impact that the wider Social Determinants have on the lives of people with serious mental illness and the importance of access to advice and support to the Mental Health Taskforce report (as part of NHSE’s Five Year Forward View). In addition, including this as one important component in a more comprehensive package of measures to help improve the lives of people living with and recovering from significant mental health difficulties, such as psychosis.
Gregor Henderson
National Lead,
Wellbeing and Mental Health
Public Health England
Comment by Chris Manning posted on
It is excellent that there is now collaborative, organised, sustained and enduring 'oomph' going into tackling the various psychotoxic source pumps of 'illth' (ill-health) in England. Far too many of our interventions are too little and too late. We can be inspired by Dr John Snow, Prof Sir Michael Marmot, Foresight Report on true Wealth (well-health) Creation and much burgeoning evidence to ACT! Our mental functions are derived from processes that are at least as physical as all our other functions; "our biology may not be our biography", yet our life prospects are far worse if our biology is severely damaged. And I know that mind is not equivalent to brain, yet there is surely some connection to what that "most complex technology in the known universe" delivers and to appreciate that our minds are embodied, as well as embrained and conjoint as well as individual. Wonderful - should ALL be centre-stage to all we do and nothing 'reductionist' about any of it. Get this emphasis right and everything else follows. I'm with you ALL the way and send my love. Chris (retired GP with lived experience of major depression)