
Welcome to the second edition of PHE’s Health Matters, a resource for public health professionals, which brings together important facts, figures and evidence of effective interventions to tackle major public health problems.
This time we are focusing on one of the most significant threats to public health in England - antimicrobial resistance (listen to the launch teleconference presentation and the Q&A featuring questions submitted by health professionals from across England).
It’s a timely topic given that many of us will be feeling under the weather during the winter months. GP surgeries will be dealing with an influx of patients asking for antibiotics to treat coughs and colds, for which they are of no use.
The pressure on healthcare professionals to prescribe antibiotics is great. But we need to conserve antibiotics and use them appropriately or we risk losing the power of these medicines.
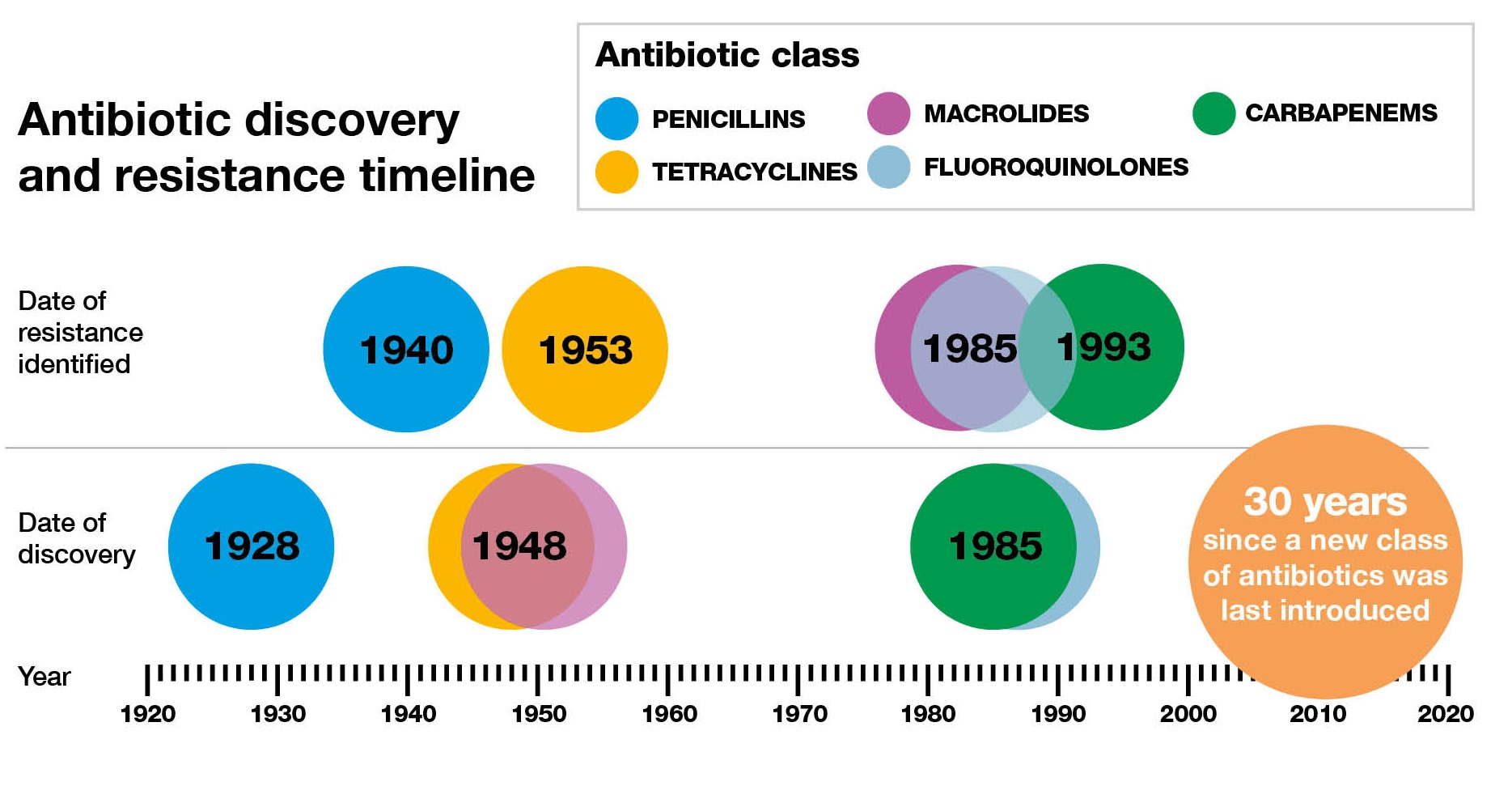
That’s because antibiotics are unlike many other drugs used in medicine, as the more we use them the less effective they become against their target organisms. With antibiotics, overuse or inappropriate use allows bacteria to develop resistance.
Antibiotic resistance occurs when an antibiotic loses its ability to control or kill bacterial growth; in other words, the bacteria become resistant and continue to multiply in the presence of an antibiotic.
We rely heavily on antibiotics. They are used to treat common infections, like pneumonia, but they’re needed for much more too. They treat infections after life-saving transplants and other surgeries, childbirth, chemotherapy, the list goes on and on.
It’s been 30 years since a new class of antibiotics was developed so we need to act now to protect the antibiotics that we have left.
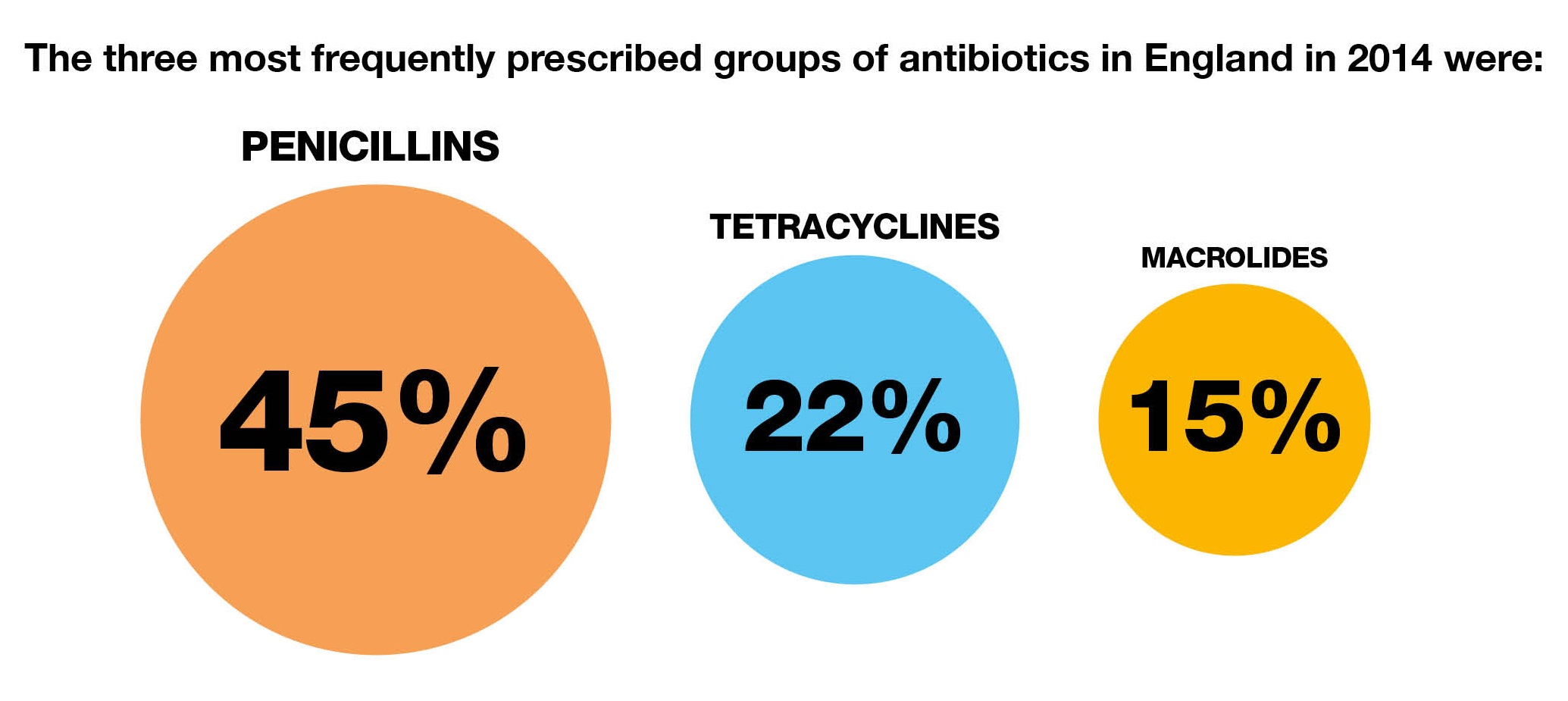
One of the ways we can do this is to cut back on prescribing antibiotics when they are not needed (see our blog on key toolkits).
Antibiotic consumption has risen by 6.5% over the past 4 years in England. We know that a large proportion of this prescribing is for sore throats, ear infections, and coughs and colds that can get better without the need for antibiotics.
This edition of Health Matters sets out the scale of the problem and how healthcare professionals, and those working in local authorities, can bring down levels of antibiotic prescribing.
The good news is that there are a number of effective ways to reduce unnecessary prescribing. Issuing a delayed prescription, for example, that the patient can use at a later date if symptoms do not improve has been shown to work. A number of other approaches are outlined in this edition.
We’ve created a suite of infographics for download that can help you make the case for implementing antimicrobial stewardship policies in your area. Antimicrobial stewardship is a cornerstone for both the effective treatment of infections and for reducing antibiotic resistance.
However, a PHE survey shows that only 18% of Clinical Commissioning Groups (CCGs) have an antimicrobial stewardship committee in place to oversee activities and promote the use of PHE’s toolkits:
- Treat Antibiotics Responsibly, Guidance, Education, Tools (TARGET) for Primary Care
- ‘Start Smart, Then Focus’ (SSTF) for Secondary Care
Only 46% of hospitals have an action plan in place to implement their Start Smart Then Focus for secondary care toolkit compared to just 13% of GP practices for their TARGET toolkit.
These figures should serve as a wake-up call. It’s clear that it’s now time for urgent action.
We simply cannot sit back and ignore the problem or we risk going back to a time where something as harmless as a cut or a scratch to the skin could claim lives.
Health Matters
Health Matters is a resource for professionals which brings together the latest data and evidence, makes the case for effective public health interventions and highlights tools and resources that can facilitate local or national action. Visit the Health Matters area of GOV.UK or sign up to receive the latest updates through our e-bulletin. If you found this blog helpful, please view other Health Matters blogs.

4 comments
Comment by Spencer Williams posted on
What about linezolid? Brought to market in 2000.
Comment by Susan Hopkins posted on
Linezolid is part of the last new class that was discovered, oxazolidinones. The oxazolidinones have been known as monoamine oxidase inhibitors since the late 1950s. In 1984, DuPont patented oxazolidinone derivatives describing their utility in treating bacterial infections. In 1987, DuPont scientists presented a detailed description of the oxazolidinones as a new class of antibiotics with a novel mechanism of action.] Pharmacia & Upjohn (now part of Pfizer) started its oxazolidinone research program in the 1990s. Linezolid was licensed by the FDA in 2000. It is important to note that acquired resistance to linezolid was reported before the drug was licensed (1999), in two patients with severe, multidrug-resistant Enterococcus faecium infection who received the drug through a compassionate use program. Linezolid-resistant Staphylococcus aureus was first reported in 2001.
Comment by Bren posted on
Hello Kevin and John,
A really timely and great blog.
My only thought is around the percentages of CCGs with antimicrobial stewardship committee in place, or, the hospital or GP Practice with action plans in place. Even if they are in place with a higher or lower figure overall percentage figure is how much they make/will continue to make a positive impact by being in place.
Just a thought and I think it is a hugely vital area in which the positive conversations around the need for action and impact will continue.
Best wishes,
Bren.
Comment by Ashley Gunter posted on
This is such an important matter, I'm glad it is finally being taken seriously.
Read a lot about the antibiotic rifaximin here http://rifaximin.co.uk