Welcome to the sixth edition of PHE’s Health Matters, a resource for public health professionals, which brings together important facts, figures and evidence of effective interventions to tackle major public health problems.
This edition focuses on preventing and diagnosing bowel cancer and encouraging more eligible people to come forward for screening (listen to the stakeholder launch teleconference presentation).
Bowel cancer, also known as colorectal cancer, is one of the most common cancers, accounting for over 10% of all cancers in England. Every 15 minutes someone is diagnosed with bowel cancer in the UK.
In 2014, it was the third most common cancer in men and women in England but the second biggest killer after lung cancer. It killed 13,036 (7,049 men and 5,987 women) in England in 2014 which is equivalent to 35 people every day.

These are frightening statistics but the good news is that bowel cancer survival is relatively good provided the disease is detected early. The earlier bowel cancer is diagnosed the better.
One year survival for those diagnosed with a stage 1 (earliest) stage cancer is 98% for men and women. When detected at stage 4 (the most advanced stage), one year survival is much lower: 44% for men and 35% for women.
Early stage cancer treatment is also significantly less expensive to the NHS than treatment for advanced disease.
The aim of the NHS Bowel Screening Programme in England, offered every two years for men and women aged 60-74, is to lower the burden of cancer in the population by discovering disease before it develops into cancer or in its early stages.
Bowel polyps are common but only around 1 in 10 will progress to potentially cancer. This progression is a slow process, generally taking about 10 years. This means there is a good window of opportunity for screening, prevention and early detection.
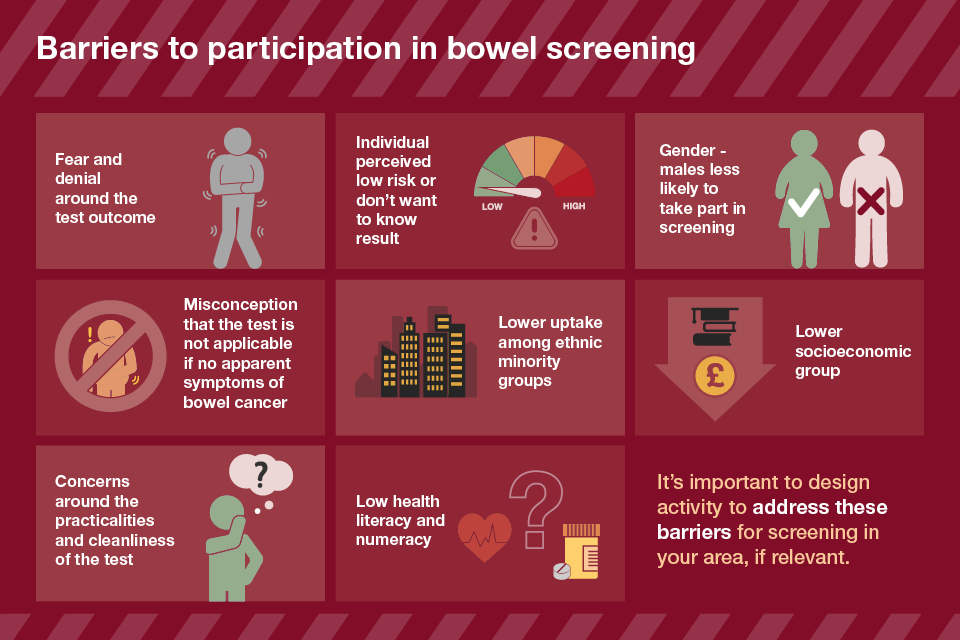
But uptake is currently not as high as it should be and below that for cervical and breast screening. The most recent uptake figure from PHE stands at 56% but in some parts of the country uptake it is as low as 33%.
PHE has a target of 75% of eligible people taking up invitations for bowel cancer screening as set out in the Cancer Taskforce Review.
The recent announcement by the government to introduce the faecal immunochemical test (FIT) in place of the existing guaiac-based faecal occult blood test (gFOBt) has been described as a “game changer” that will help to boost screening uptake by around 10% - meaning an additional 200,000 people could be tested each year.
More information on how FIT will increase uptake as well as other methods for boosting screening uptake, such as GP participation letters, are outlined in this edition of Health Matters.
This edition also contains information on the lifestyle changes that can play a key role in reducing the chances of developing bowel cancer in the first place.
Local authorities have responsibility for commissioning behavioural and lifestyle campaigns to prevent cancer.
These should highlight that the risk of bowel cancer can be reduced by:
- exercising regularly
- stopping smoking
- reducing the amount of alcohol consumed
- maintaining and achieving a healthy weight
Read the bowel cancer edition of Health Matters for more on what local authorities and health professionals can do to reduce the number of deaths from cancer’s second deadliest cancer.
Health Matters
Health Matters is a resource for professionals which brings together the latest data and evidence, makes the case for effective public health interventions and highlights tools and resources that can facilitate local or national action. Visit the Health Matters area of GOV.UK or sign up to receive the latest updates through our e-bulletin. If you found this blog helpful, please view other Health Matters blogs.

1 comment
Comment by Jona posted on
There is definately a great deal to know about this issue.
I love all of the points you've made. http://www.yahoo.net