I hope you've seen that we recently published a new edition of Health Matters, focusing on improving the prevention and diagnosis of bowel cancer.
PHE, through the National Cancer Registration and Analysis Service (NCRAS), collects and analyses the data on how all cancers affect the population and, as such, have been able to track changes in bowel cancer over time.
Bowel cancer is one of the most common cancers, accounting for over ten percent of all cancers in England.
In 2014 it was the third most common cancer in men and women but the second biggest killer after lung cancer. It killed 13,036 (7,049 men and 5,987 women) in England in 2014 which is equivalent to 35 people every a day.
While incidence (the number of new cases of bowel cancer diagnosed each year) has historically gone up, death rates have been falling since the 1970s as treatments and early diagnosis has improved.
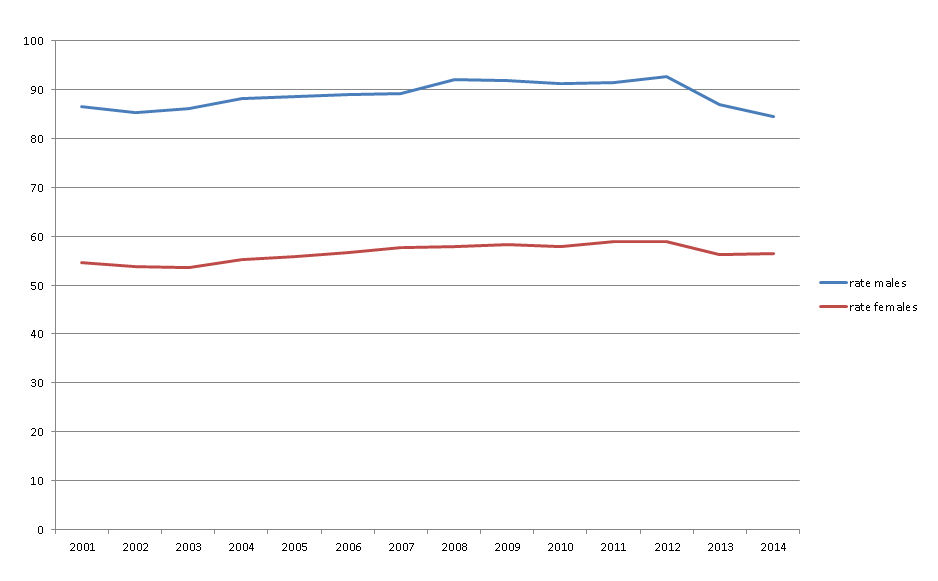
The graph below shows that this gradual increase continues until 2012, when it starts to decrease for both men and women. The drop in incidence since 2012 is an interesting point for further discussion and investigation.
The importance of early diagnosis
Early detection is fundamental to short and long-term survival. The earlier bowel cancer is diagnosed the better.
One year survival for those diagnosed with a stage 1 (earliest) cancer is 98% for men and women. When detected at stage 4 (the most advanced stage), 1 year survival is much lower: 44% for men and 35% for women.
Cancers can be diagnosed from a number of different routes. Often this is through screening or when a GP refers someone when they present with symptoms. Sometimes, however, cancer is diagnosed as a result of an emergency presentation.
Cancer is more likely to be detected at an early stage via screening or via a 2 week wait GP referral. It is more likely to be diagnosed late when it’s diagnosed as an emergency presentation. I will discuss routes to diagnosis later in the blog.
Screening and colonoscopy
Currently people are screened via a FOBt test and if that’s positive they are called for a diagnostic test which is usually colonoscopy. As well as finding cancers, the colonoscopy can find adenomas (premalignant growths that turn into cancers) and, if removed, this can stop cancers forming in the first place.
The FOBt home screening test is gradually being replaced by the new FIT test, which is more effective at detecting blood in poo so should lead to more cancers being found through screening. But colonoscopy is also important as the more adenomas that can be found and removed the more cancers can be prevented.
Routes to diagnosis
NCRAS has also used the latest available data to produce an extensive set of results for over 2 million patients and how they were diagnosed with cancer between 2006 and 2013. This work is called Routes to Diagnosis and has been important in measuring and driving improvements in early diagnosis.
For all cancers the proportion diagnosed through an emergency route has decreased from 24% to 20%, whilst the proportion of cancers diagnosed through urgent GP referral with a suspicion of cancer, the Two Week Wait route, has increased from 25% to 34%.
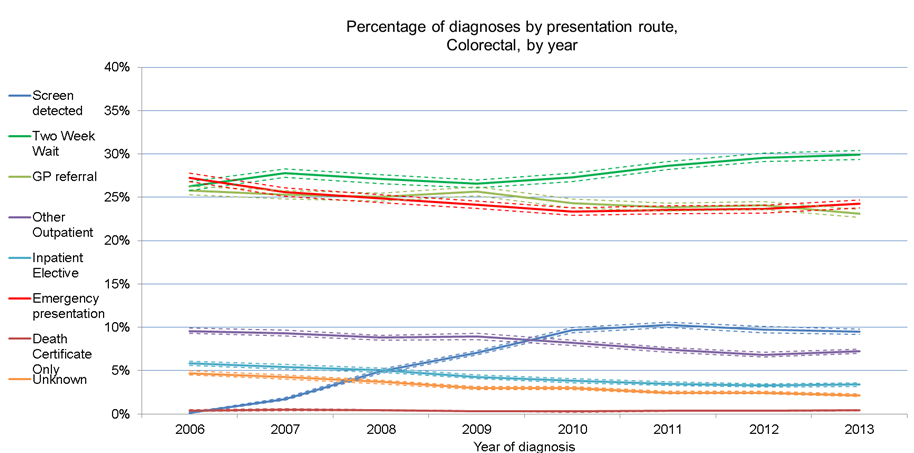
As mentioned, bowel cancer is unique to other cancers in that it has a screening programme for men and women. In 2013 9% of bowel cancers were diagnosed through screening, 30% through two week wait, 23% through GP referral and 24% by emergency presentation.
The graph shows us how early diagnosis has improved for bowel cancer since 2006.
The latest figures also clearly show the impact of the roll out and age extension of the bowel cancer screening programme.
Our motivation lies within the rich detail that the results are able to give us, and in the variation and inequalities that our data continue to reveal.
For people with colorectal cancers, only 7% in the most deprived areas are diagnosed through screening compared to 11% in the least deprived areas.
Too many people with cancer are still being diagnosed too late. We have a responsibility to utilise the cancer data that we are entrusted with to ensure that we are doing all that we can to help understand why this is and what can be done to make a difference to patients.
Health Matters
Health Matters is a resource for professionals which brings together the latest data and evidence, makes the case for effective public health interventions and highlights tools and resources that can facilitate local or national action. Visit the Health Matters area of GOV.UK or sign up to receive the latest updates through our e-bulletin. If you found this blog helpful, please view other Health Matters blogs.