The Evidence Review for UK’s second Climate Change Risk Assessment was published recently by the Climate Change Committee, having been developed by literally hundreds of authors, reviewers and stakeholders.
There’s a wealth of information and analysis available within it, helpfully summarised in a key messages leaflet, animation (above) and slides.
The entire review will now be considered by government and used to develop the 2nd UK Climate Change Risk Assessment and National Adaptation Programme, as set out in the Climate Change Act 2008.
The review goes beyond previous work because; not only does it set out the major risks the UK faces from climate change this century, but crucially it also identifies the 6 priorities for action and research in the next 5 years, accounting for what is already being done.
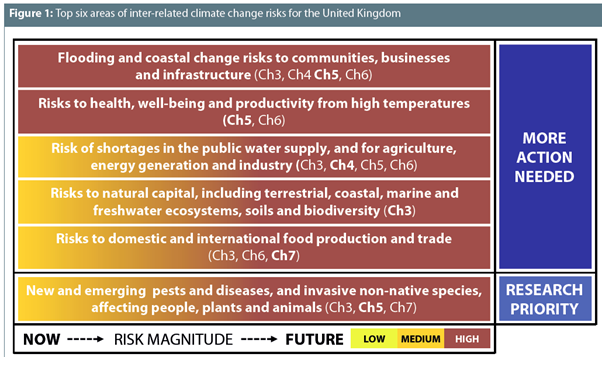
The scale of the challenge
So what does this mean for public health? Firstly, this review reminds us of the scale of the challenge.
Our climate has already changed and will continue to do so; the question is by how much? If the world meets the carbon emission reduction commitments made in Paris in 2015, we expect an increase in mean global surface temperature of 2.7°C by 2100.
If we don’t, 4.1–4.8°C is possible, with a 6°C rise plausible. To set this in context, global surface temperatures were 6°C cooler than today during the last glacial period (‘ice age’); the converse seems unimaginable to me.
Whilst we are already committed to a certain degree of climate change and must prepare and respond to it, carbon reduction (with all its potential health benefits) must remain our primary objective.
We're all in this together
Secondly, the review recognises the interdependency of risks and our responses, and acknowledges that what happens in the rest of the world will affect us in the UK (eg through disruption of trade/supply chains).
We are definitely ‘all in this together’ whether we like it or not. Whole system approaches are needed, as success or failure of any other part of the system, such as agriculture, infrastructure and our economy, will influence our health and wellbeing.
Public health professionals are integral, through providing real world approaches to needs/asset assessments and evaluation of complex interventions, and can be important advocates for action.
Tackling heath inequalities and the burden of non-communicable disease share many of the same challenges and underlying causes, and we should consider how meeting these challenges together could magnify positive, and diminish negative outcomes.
Focus on priority areas
Thirdly, the review helps move us from describing a problem of almost paralysing proportions and complexity, to focusing on key priority risks that we can, and must, act upon now.
Chapter 5 details these risks particularly from the health perspective, with flooding, high temperatures, and health and social care service delivery, identified as areas where there is a high level of current and future risk and more action is needed.
Areas with significant research gaps include viability of coastal communities, impact on health from changes in air quality, emerging diseases and the impact of adaptation strategies on vectors.
Some benefits have been identified, such as a small reduction in cold-related mortality and recreational opportunities afforded by warmer weather, but these are heavily outweighed by the risks.
Let’s take just one example: high temperatures and their impact on health. Our warming climate and an ageing population mean that heat will pose an increasing threat in the UK in the years to come.
Although the Heatwave Plan for England has likely had some impact in reducing heat related illness since 2004, future effects are likely to be more pronounced.
Overheating of homes, hospitals and care homes is of increasing concern, and more emphasis is needed on improving homes and other buildings to keep occupants cool in summer, whilst continuing to make energy efficiency and other improvements to address health risks posed by cold homes in winter.
The review reminds of the scale of the risk, the need for whole system approaches and helps us focus on the most urgent problems to tackle.
The challenge for us is whether the evidence presented will persuade us to act at the scale and pace needed. The longer we leave it, the greater the challenge we leave ourselves, others (especially in low income countries) and future generations.
It’s so easy to feel overwhelmed or jaded and to make excuses. When I find myself doing this, I imagine a future conversation with my grandchildren. Telling them that I didn’t know the risks, or what to do, that there was too much else to do, or that it was someone else’s responsibility, just won’t cut it.

2 comments
Comment by simon posted on
Enjoying al climate change articles, as is a concern for public health. Would like to see an article on how we could measure or project any potential local impacts ?
In the past we have tried looked at linking weather data to our mortality and hospital activity, but sadly the MET office charges for such information so we were unable to do this. Are there any other sources of weather data we can freely access ?
Comment by Guest posted on
Thanks so much
https://oto1s.com