
Earlier this month we hosted our fifth annual cardiovascular disease (CVD) prevention conference – Getting Serious About CVD Prevention 2018 – with a focus on the world leading NHS Health Check.
This year’s conference was attended by over 450 delegates from across the country. The day was dynamic, consisting of presentations from key delegates in the field, 12 workshops including roundtables and interactive discussions, panel discussions and Q&As, and a lively balloon debate. All of the conference presentations are available online.
Why do we host this conference?
CVD remains a leading cause of disability and death in the UK, where it affects around 7 million people and is responsible for 1 in 4 premature deaths.
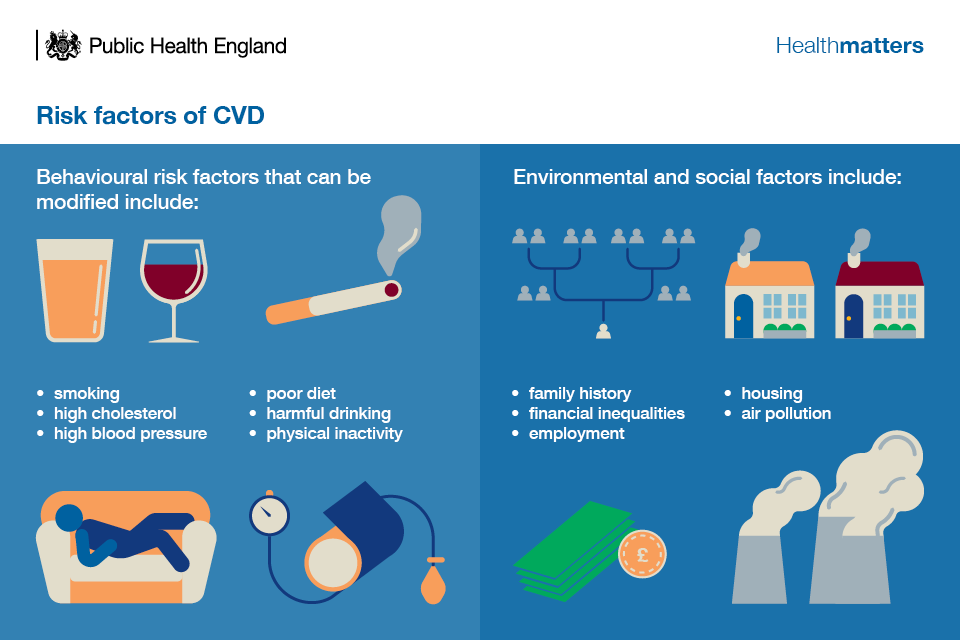
However, 50% to 80% of CVD cases are preventable, as they’re largely caused by modifiable risk factors including high blood pressure, physical inactivity, smoking and obesity. With these risk factors being more prevalent amongst lower socioeconomic groups, CVD is one of the conditions most strongly associated with health inequalities. It also places a considerable strain on the NHS and wider society, accounting for an estimated £8.96 billion a year in NHS healthcare costs alone.
Continued efforts towards preventing CVD and closing the health inequality gap are evidently crucial, but this is a huge task that cannot be achieved by one organisation or discipline alone. As such, this conference brings together the many professions and organisations required to collaboratively tackle this challenge, including academics, providers, commissioners, government, the third sector and commercial organisations. .
What was this year’s key message?
This year’s focus was on ‘reducing variation and optimising care’, which persisted as the strong underpinning message of every session throughout the day.
Across England, there is variation in NHS Health Check offers and uptake; depending on where you live, you are more or less likely to be offered and take up a Check. Each of the speakers emphasised the great impact the programme has on CVD prevention, and the importance of maximising its potential by ensuring 100% of the eligible population receive an offer for the Check.

The presentations and workshops focused on the following areas that must be addressed to improve CVD prevention and boost uptake of the NHS Health Check.
Tackling CVD together with an integrated approach
The power of tackling CVD together, and having the humility to recognise that we need each other, was the message Duncan Selbie relayed to the audience to commence the day. PHE’s CEO also stressed that the programme was here to stay and had become a cornerstone for our prevention activities in tackling non-communicable diseases in England.
Closing the inequality gap
The health inequality gap is a significant issue for CVD, as it makes poverty the determinant of your outcome if you have, or are at risk of developing CVD. The severity of this inequality gap and the need to close it was reiterated throughout the conference.
Professor Kevin Fenton, Director of Public Health for the London Borough of Southwark, spoke about the significant differences in healthy life expectancy between the poor and affluent. He shared that in Southwark, mortality rates from CVD are higher than regional and national averages, reflecting its status as one of the most deprived boroughs in all of England.
The NHS Health Check is available for all individuals aged 40 to 74, so we must work to ensure that the invitation is sent out to and accepted by all those eligible, regardless of socioeconomic status or their borough’s deprivation level.
Using data, innovation and different approaches
Many of the speakers across a range of professions and organisations focused on driving improvement in CVD prevention by doing things differently. In a workshop dedicated to this topic, Dr Matt Kearney, GP and National Clinical Director for CVD Prevention in NHS England and PHE, gave us a GP’s perspective by saying that it’s not about GPs working harder, but doing things differently to support GPs to get better and detecting and managing CVD.
Ged Devereux from the Cheshire and Merseyside Fire and Rescue Service (CFRS) spoke about his team working outside of their silos for the good of all the people they serve in Halton CCG. As part of their Safe and Well visits, the CFRS are screening for Atrial Fibrillation (AF) to identify the estimated 500 people who have undiagnosed AF and signpost them to appropriate follow-up management.
Follow-up management after identifying individuals at risk
Optimising care and ensuring individuals identified as being at CVD risk receive follow-up management were also key messages underpinning each session throughout the day.
Specific actions that were highlighted included:
- having effective and relevant interventions in place
- linking individuals in need of follow-up management to behavioural change programmes
- using public health resources effectively to have a seamless and streamlined process to help manage people with CVD
As set out in the NHS Five Year Forward View, PHE will work with STPs and NHS England including RightCare to support implementation of interventions.
Read our recently published Stocktake and Action Plan and latest edition of Health Matters to learn more about the priority areas for action over the next 5-year cycle of the NHS Health Check and what you can do to reduce variation and optimise care.
