
We have now published the first update to our Health Profile for England, a report which gives the most comprehensive picture of the health of the population.
When we published last year’s report, it was the first time we had presented our population health data in a way that told a story. Now, just over a year on, we have updated the data and developed this to include a chapter looking at child health, as well as future trends, forecasting what the story might look like in years to come.
In this blog we look at these forecasts, as well as what we have learned about how morbidity is shifting and how the wider determinants of health are having a big impact.
What are the future forecasts telling us?
Right now life expectancy in England is 79.6 years for men and 83.2 for women. The population is increasing and people are living longer, which means society is changing and our health is changing with it. The new report tells us that the number of people aged over 85 will hit more than 2 million people by 2031.
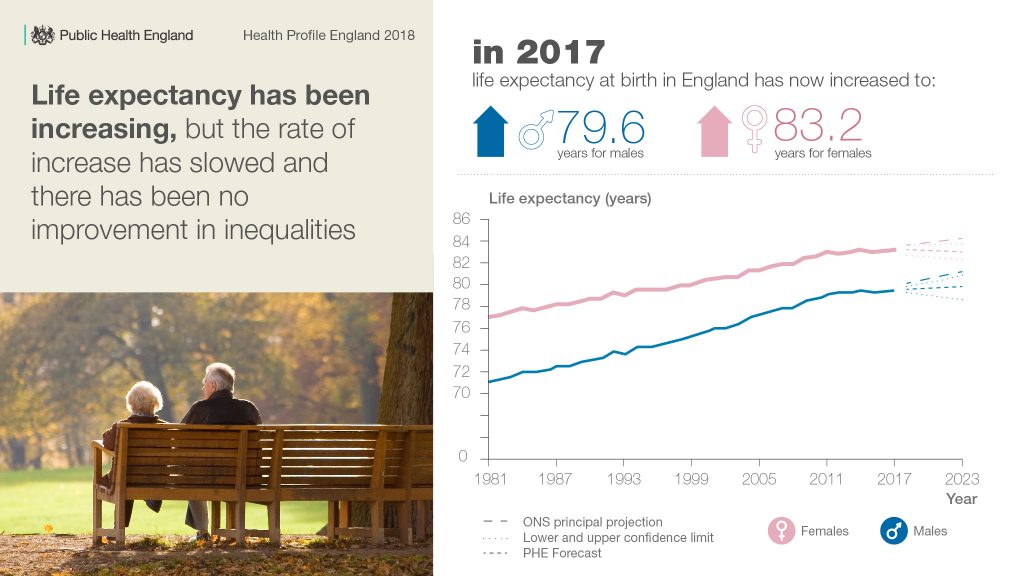
Although our lives are getting longer, stubborn health inequalities persist across the country and it remains the case that people in the richest areas enjoy 19 more years in good health than those in the poorest.
Having an ageing population means that the number of people with long-term health conditions, many of the most common of which are preventable, has increased. They play a major role in inequalities and on the burden felt by the NHS, accounting for 70% of total health and social care spending in England.
For example cases of type 2 diabetes, which costs the NHS a staggering £8.8 billion to treat each year, are projected to rise by a further one million people by 2035. This means that there will be almost 5 million individuals in England with this largely preventable disease, which can also cause sight loss, kidney disease, amputations, heart disease and stroke.
Dementia and Alzheimer’s disease is already the biggest cause of mortality in women, and the report forecasts that the death rate may overtake heart disease and therefore it is likely to become the leading cause of death among men too. This could happen as early as 2020 and while the reasons for this are not clear, increased awareness of dementia, making it more likely to be diagnosed and recorded, is clearly a factor.
How is morbidity shifting and what does this mean?
Age-specific morbidity rates (the number of people with certain diseases per 100,000 population) have decreased for all age groups between 1990 and 2016, however as our population ages, morbidity reasons are shifting.
The Health Profile tells us that we are actually now healthier at every age group, however the number of people with a long-term condition is likely going to keep rising, and this doesn’t just mean conditions such as diabetes and cardiovascular disease.
Low back and neck pain as well as skin diseases (mainly dermatitis, acne and psoriasis) remain the two leading specific causes for morbidity for both males and females. Hearing and sight loss are also now ranking highly as morbidity causes for both sexes.
With these conditions on the rise, it’s vital that the NHS can diagnose and treat them adequately. Addressing this means a big change in how the system works, compared to the way the NHS was set up and has treated patients for many years.
We also know that women’s health is fairing worse than that of their European counterparts compared with men, ranking just 18th for early death, whereas men are ranked 10th.
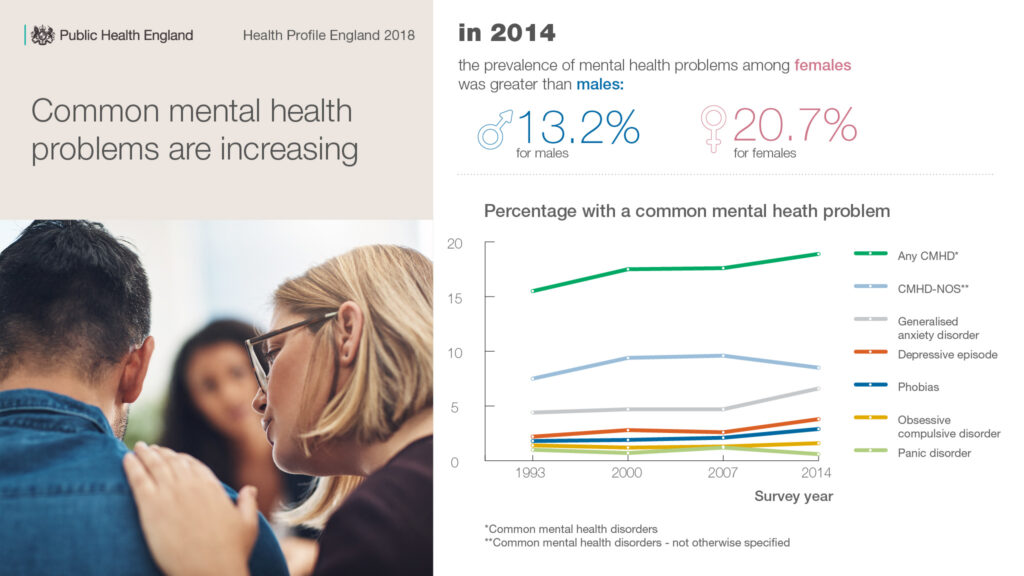
The causes of morbidity become more prevalent with age, but the profile shows that mental health problems and substance use have the biggest effect on younger adults, accounting for a third of disease burden on those aged 15 to 29 years.
What role are the wider determinants of health playing?
The morbidity causes mentioned above can have extremely negative impacts on people’s lives, but health is about much more than healthcare and the services we use when we are unwell.
For most people, the ingredients for a healthy life are relatively straight-forward: a good education, a good job, a suitable roof over your head and people to care for and about. When these factors are falling short of a decent standard, health can suffer.
The report tells us that nearly 30% of people in the UK are living below the Minimum Income Standard, which is based on what the public think we need to achieve a decent standard of living. This percentage is even greater among children (44.3%) than working age adults (29.0%) and pensioners (15.4%), which is concerning, as having the best possible start in life is an important factor in determining an individual’s future health and wellbeing.
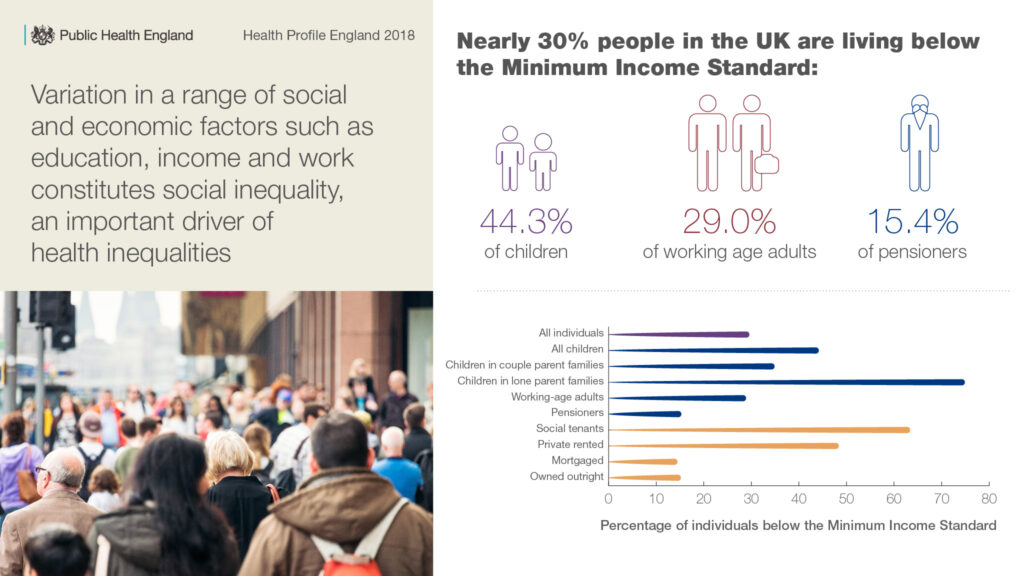
Having a decent job is a vital part of this, but access to employment varies drastically for people with certain limiting health conditions. Only 5.7% of people with a learning disability and 7.0% of people in contact with secondary mental health services are in employment.
Of course our employment affects the kind of home we have and right now in England, 20% of dwellings, amounting to 4.7 million homes, are failing to meet the Decent Homes Standard.
These things go hand in hand with good health and are very much the basis of a person’s life, so the more we see improvements in the number of people in decent homes, with decent employment, the more improvements we will see to overall health and wellbeing.
Find out more about the Health Profile for England in our 10 facts about the health of the nation blog.
We want the data from the profile and the narrative of the story it tells to be used by decision makers to play a role in creating policies. Download the graphs and infographics and use them to inform constructive conversations about the health of people both locally and nationally.

2 comments
Comment by J Burrage posted on
is anything taken into consideration about the ill health of people caring for family members who've long term health problems and the impact this has on there own health and life expectancy
Comment by Karen clarke posted on
I think we all have health issues and anyone caring should not be overlooked or overlook theirs. They themselves should not be complacent and should be given breaks and consideration too.