
The latest edition of Health Matters, PHE’s professional resource, focuses on the new ambitions developed by the Cardiovascular Disease Prevention System Leadership Forum (CVDPSLF) that sets to improve the detection and management of atrial fibrillation (AF), high blood pressure and raised cholesterol, and reduce the health inequalities associated with CVD, over the next 10 years.
This blog provides a summary of the full edition’s content.
CVD is the leading cause of death worldwide
As the leading cause of death worldwide, CVD accounts for 17.9 million lives each year, which is 31% of all global deaths. Poor cardiovascular health can cause heart attacks, strokes, heart failure, chronic kidney disease, peripheral arterial disease, and the onset of vascular dementia.

Falling mortality rates from heart disease were the biggest cause of increases in life expectancy between 2001 and 2016 in England, according to PHE’s Health Profile for England. However, since 2011 the rate of increase in life expectancy has slowed for both sexes as improvements in heart disease mortality have plateaued. This highlights the need for a renewed drive to prevent CVD deaths, which still account for one in four of all deaths in England; the equivalent to one death every four minutes.
Although CVD mortality rates have almost halved over recent decades, there is no room for complacency in the efforts required to address the major challenges that CVD continues to play in individual lives, communities and society as a whole.
CVD morbidity is also a major issue for health and social care as 6.8 million people are living with cardiovascular conditions. This places a considerable financial burden on the NHS and wider society, with CVD-related healthcare costs alone in England amounting to an estimated £7.4 billion per year, and annual costs to the wider economy being an estimated £15.8 billion.

Furthermore, CVD is one of the conditions most strongly associated with health inequalities. If you live in England’s most deprived areas, you are almost four times as likely to die prematurely than those in the least deprived. CVD is also more common where a person is male, older, has a severe mental illness, or ethnicity is South Asian or African Caribbean.
Addressing secondary prevention – the new national ambitions
Given that the majority of CVD cases are preventable, there is huge opportunity to make a difference in improving CVD outcomes.
Whilst primary prevention projects form a significant part of NHS England’s and PHE’s ongoing work to tackle CVD, there has been an absence of co-ordinated action to tackle the secondary prevention of CVD to date.
The recently published NHS Long Term Plan includes a major ambition to prevent 150,000 strokes, heart attacks and dementia cases over the next ten years. To complement this, the National CVD CVDPSLF has agreed specific ambitions for the detection and management of the high risk conditions:
- Atrial fibrillation (AF)
- High blood pressure
- High cholesterol
These common conditions can cause CVD, including heart attacks and strokes, and many cases of dementia. Although treatment of these conditions is very effective at preventing cardiovascular events, late diagnosis and under treatment is common.
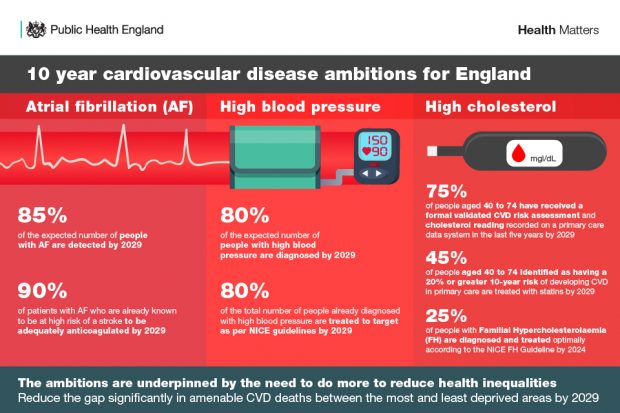
Independent PHE estimates show that if the ambitions are met, at least 49,000 strokes and 31,000 heart attacks could be prevented. Other events averted include heart failure, transient ischaemic attacks, vascular dementia and angina.
Achieving the ambitions
Achieving the ambitions requires a whole system effort. Whilst in the past, primary care has been thought of as responsible for identifying CVD risk factors, it is being overstretched and there are many other ways of finding the people most at risk.
This edition of Health Matters provides calls to actions for local authorities, clinical commissioning groups, general practice, pharmacists and community settings, including:
- using the NHS Health Check to support early diagnosis and management
- implementing NHS England’s RightCare CVD prevention pathway
- using existing data to make the case for action
- making positive behavioural changes for preventing CVD
- raising public awareness of CVD risk factors and opportunistic detection
Fundamental to achieving the ambitions is also the need to drive reductions in the gap in avoidable CVD mortality and morbidity between the most and least deprived. As, PHE analysis shows that 40% of amenable CVD deaths occur in the three most deprived deciles in England, over 40% of action of all ambitions should be delivered to these deciles to prevent the gap from widening further.
It has been a privilege to chair the CVDPSLF, which now includes representation of over 40 different members, including statutory organisations, the third sector, royal collages, academia and expert public voices. Over the coming months and years will continue to work together to support delivery of these important ambitions, including publishing our individual and shared commitments and highlighting how the whole system can support England to be word leading in the prevention of CVD, which we know still negatively impact lives of millions of people, often living in our more deprived communities
Visit the Health Matters area of GOV.UK or sign up to receive the latest updates through our e-bulletin. If you found this blog helpful, you can read other Health Matters blogs.

2 comments
Comment by Tim posted on
A recent study published in The Lancet found "The population attributable fraction of the concentration of lead in blood were
28·7% (15·5–39·5) for cardiovascular disease mortality
37·4% (23·4–48·6) for ischaemic heart disease mortality".
The last time blood lead levels were surveyed, 27% of toddlers had lead toxicity.
Why are you not trying to reduce lead exposure as they do in the USA?
https://www.thelancet.com/journals/lanpub/article/PIIS2468-2667(18)30025-2/fulltext
Comment by Dorothy posted on
It's very interesting to read about these projects. I think that they should be implemented in all local areas, Coventry for example, as a lot of young people have lost their lives this year through HBP.
More awareness needs to be made locally to reduce the level of death that occurs every month in relation to this cardiovascular disease.
Well done for how far you've gone and would go on this prevention program.