
Being deployed into an international disease outbreak situation is a reasonably stressful experience.
The stress starts the minute you get the call to leave; how big is the outbreak? What’s the pathogen? How dangerous is the living and working environment? Should I pack my Aeropress? Questions that all pale into insignificance when you’re explaining to your kids why you’re flying to a distant country with ‘a really nasty disease that’s killing lots of people’.
But stress and excitement are a hairs width apart, and deploying to an outbreak can also be an incredibly rewarding, challenging and humbling experience and for me it’s an opportunity to make a tangible difference in the world.
Being ready to deploy anywhere in the world
Having to be ready to deploy anywhere in the world within 48 hours means that occupational health have you jabbed up against every possibly nasty they can think of. Most of the pathogens we deal with don’t have vaccines but these jabs help rule out the obvious ones if we were to get sick whilst abroad.
The logistics team have issued all deployable staff with suitcases and grab bags full of items that make life easier when operating in a fragile or difficult environment. These include things like multi region Wi-Fi dongles, indestructible smartphones, state of the art mosquito nets and a little orange whistle. My kids like to imagine these gadgets get handed out to me by some Q-like figure in a Bond film.
When the call comes to deploy, the UK Public Health Rapid Support Team (UK-PHRST) Operations team spring into action and send out pre-deployment briefings that include any and all details about the country we are deploying to, the pathogen, the outbreak status, the response and any security, political and logistical information that we might need.
Flights are booked, accommodation is secured in Foreign Office approved, security vetted hotels and transport arrangements in-country are planned.
One of the more unsettling aspects of a deployment for family members is that we never know how long we will be gone, it could be two weeks but it could be six depending on the situation we find, the span of the outbreak and our ability to make a difference to the response whilst there.
The role of Field Logistician
My job as Field Logistician for the UK Public Health Rapid Support Team is broadly twofold; to provide the logistical support to the wider team, hopefully allowing them to do their jobs more effectively and to provide technical logistics advice and training to host governments on outbreak logistics.
Supporting a team of epidemiologists, clinicians, data scientists and microbiologists to ensure they have adequate transport, security, accommodation, communications and field support whilst in an outbreak in a developing country can be likened to herding squirrels whilst riding a unicycle blindfolded.
It is not an easy job and can frequently be one that doesn’t go to plan, but this is all part of the work.
My background and training were originally in existential psychotherapy, the treatment of complex drug and alcohol addictions and the commissioning of city wide addiction services, so I have much experience of dealing with what could be chaotic situations and heavy workloads.
When the opportunity arose to volunteer and head to Sierra Leone in 2014/15, during the Ebola outbreak, I jumped at the chance and started working in the Kerrytown Ebola treatment centre under the guidance of PHE’s Neil Bentley (who’s fascinating career you can read more about here).
Neil recognised that the lab supply chain, was causing significant issues for the PHE teams working in all of Sierra Leone’s labs, as they were running out of essential items to run diagnostic tests and were having to use often inadequate personal, protective equipment. Neil tasked me with coming up with a logistics plan to remedy the situation.
The problem was that there were too many links in the supply chain, too many people getting involved in the ordering and shipping process and high staff turnover in the labs. This meant that often orders got lost along the way and nobody could remember who ordered what.
I designed a simple, single point of contact system for the labs to complete all orders and track shipments. Four years later I am still working on supply chain issues in outbreak situations.
Supporting the Nigerian Government through a Lassa Fever outbreak


In February 2018, the UK-PHRST sent a small team to support the response to a larger than normal Lassa fever outbreak in Nigeria.
The team consisted of two epidemiologists, a clinician and myself as the Field Logistician. As this was a ‘bi-lateral’, government to government deployment, which means one government working alongside another, logistical arrangements were the responsibility of the Rapid Support Team.
In bilateral deployments like this one, the UK-PHRST adheres wherever possible to Foreign and Commonwealth Office (FCO) guidelines for UK civil servants travelling and working abroad.
For the Nigeria deployment we arranged logistical support in the form of transport and local procurement through the African Field Epidemiology Network (AFENET), who continued to support us throughout the duration of our stay.
Challenges during the deployment
Having the dual remit of providing team support and technical advice in Nigeria presented a number of challenges. One day I was conducting field visits, investigating supply chain issues in the Irrua and Owo Lassa treatment centres where we were witnessing the highest concentration of patients, and the next day I was spending several hours procuring local SIM cards in Abuja for the team to use in their deployment phones.
Something as simple as buying a SIM card, which in the UK would take 5 minutes to procure, requires official registration in Nigeria and you have to take your passport and wait in an extremely long queue before filling out multiple forms and finding out that you can only procure 3 SIMs per day so will need to do it all again tomorrow.
Without local SIMs the team cannot operate and communicate, both with each other and with the local NCDC experts on the ground. The local SIMs also allow us to use our global dongles and have roaming internet and access to emails which is vital in fast moving outbreak scenarios.
The coordination of transport in these situations is always a minefield and we need to make plans for several people, often wanting to go in different directions, at different times and to meetings that are invariably vitally important.
In Nigeria this also meant coordinating internal flights, making sure we had cars and drivers to meet us in remote locations and ensuring that local hotels were safe and appropriate to our needs. The key to success in field logistics is to ensure that your team communicate their needs effectively and in a timely manner. Failure to plan in an outbreak, in a challenging environment, can have unforeseen and potentially catastrophic consequences.
The uninterrupted supply of personal protective equipment (PPE) and medicines was a particularly challenging issue during the outbreak and there were ‘stock outs’ in a number of locations, requiring emergency action by the World Health Organisation (WHO). This essentially means none left to hand out to people.
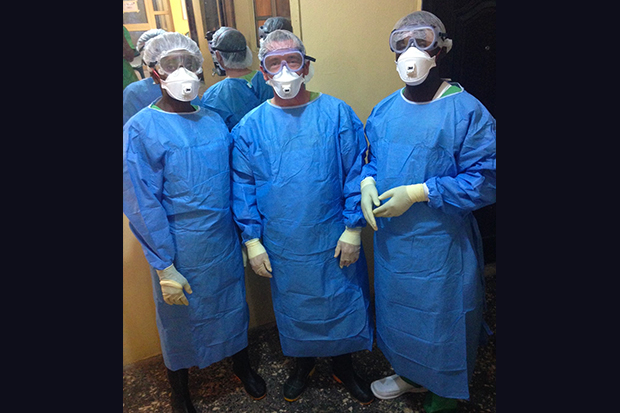
A stock out of vital PPE could force front line staff into unsafe practices such as reusing gloves or gowns that have the potential to spread disease, which is something we have to stop from happening.
Training others
Since the deployment we have worked closely with the Nigeria Centre for Disease Control (NCDC) to develop a package of training to upskill local logisticians in the importance of maintaining effective supply chain management in an outbreak situation.
In March 2019 three members of UK-PHRST staff delivered a two day ‘train the trainer’ event that was well attended by six different states and a number of NCDC logistics staff. All attendees committed to take the materials presented by NCDC, UK-PHRST and WHO representatives, and use it to train front line staff on the importance of stock management and supply chain in outbreaks.
The event also allowed the opportunity for laboratory staff from the National Reference Lab to address their own logistical concerns and seek ongoing support to ensure effective supply chains for diagnostic services.
The opportunity to work on capacity building training and follow up with local staff to implement the changes they identify has been a hugely rewarding facet of the job. It has helped identify new areas that the UK-PHRST can support NCDC in driving forward meaningful change on the front line of logistical support and supply chain management.
If you liked this blog, you can read more from our Disease Detectives series by clicking the links below:
Using supermarket loyalty cards to trace an E Coli outbreak
keeping track of new and emerging infectious diseases

1 comment
Comment by easybuilder.pro posted on
lack of transparency in that area..