
This is the latest in a series of blogs summarising what we learn each time we update the Public Health Outcomes Framework (PHOF). The latest update includes 8 indicators, some of which we explain below.
The PHOF includes a set of indicators that help us understand how well public health is being improved and protected. It aims to reflect a focus not only on how long people live, but on how well they live at all stages of life.
Antibiotic prescribing in primary care has continued to decrease
Antimicrobial resistance is a global public health issue, driven by the overuse and inappropriate use of antibiotics, antivirals and antifungals. It can mean that standard treatments become ineffective causing infections to persist and possibly spread to others. One of the key areas of action to prevent the post-antibiotic era is to reduce the use of inappropriate antibiotics. In England, Clinical Commissioning Groups (CCGs) were incentivised through the Quality Premium (QP) scheme to reduce antibiotic use in their population.
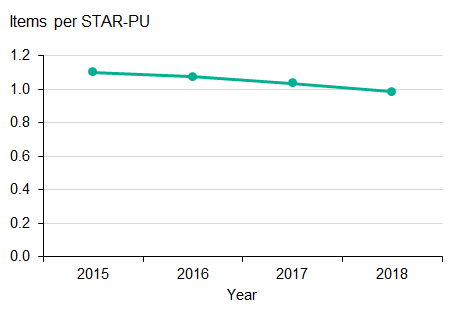
Antibiotic prescribing in primary care is measured as an age and sex adjusted metric of items per STAR-PU (Specific Therapeutic group Age-sex weightings Related Prescribing Unit), which allow for more accurate comparisons of prescribing between different geographical areas. The lower the value, the fewer prescriptions were given per head of population.
For the 2017/18 financial year, the QP target was a prescribing rate equal to or below 1.161 items per STAR-PU (the mean value for England in 2013/14). The benchmark for the ‘adjusted antibiotic prescribing in primary care by the NHS’ indicator is aligned with the QP. Overall, the rate of antibiotic prescribing in primary care in England has reduced by 10.0% (from 1.10 STAR-PU in 2015 to 0.99 in 2018), with ambitions to reduce prescribing further as set out in the UK AMR five-year National Action Plan.
Completion of treatment after 12 months for Tuberculosis (TB) has remained stable, while incidence declined
Two indicators in the health protection domain have been updated with 2018 data following the recent publication of the Tuberculosis in England 2019 report.
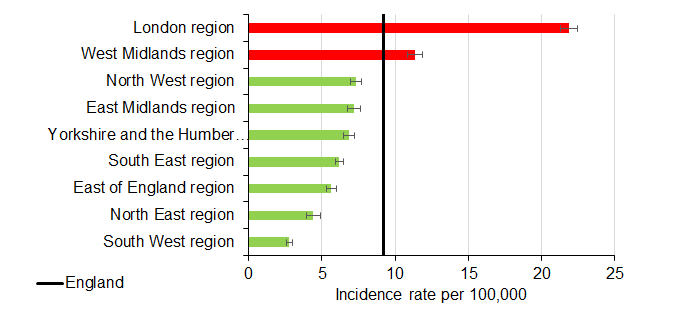
At a national level, TB incidence continues to fall. TB incidence in England for 2016 to 2018 was the lowest ever recorded at 9.2 cases per 100,000 population. The burden of the disease varied across the country and remains concentrated in large urban areas; London had the highest rate at 21.9 cases per 100,000 population.
The proportion of people with drug sensitive TB who completed treatment by 12 months in 2017 (84.7%) remained similar to 2016 (85.0%). As with incidence, there is variation by geographical region. The North East had the lowest proportion completing treatment in 2017 (74.7%) while Yorkshire and the Humber had the highest treatment completion (88.9%).
The estimated dementia diagnosis rate (EDDR) has remained stable
An early diagnosis of dementia enables people living with dementia, their carers and healthcare staff to plan accordingly and work together to improve health and care outcomes. A diagnosis rate of two thirds of the estimated people with dementia was set as a target following the Prime Minister’s dementia challenge 2020.
The estimated dementia diagnosis rate (aged 65+) was created to help inform decision making and measure progress against the target rate. It is calculated using the number of people with a recorded diagnosis of dementia within the population divided by the estimated number of people living with dementia. These estimated number of people living with dementia are determined by the results from the Cognitive Function and Ageing Study II (CFAS II). More information on the study can be found at the following link: https://www.sciencedirect.com/science/article/pii/S0140673613615706.
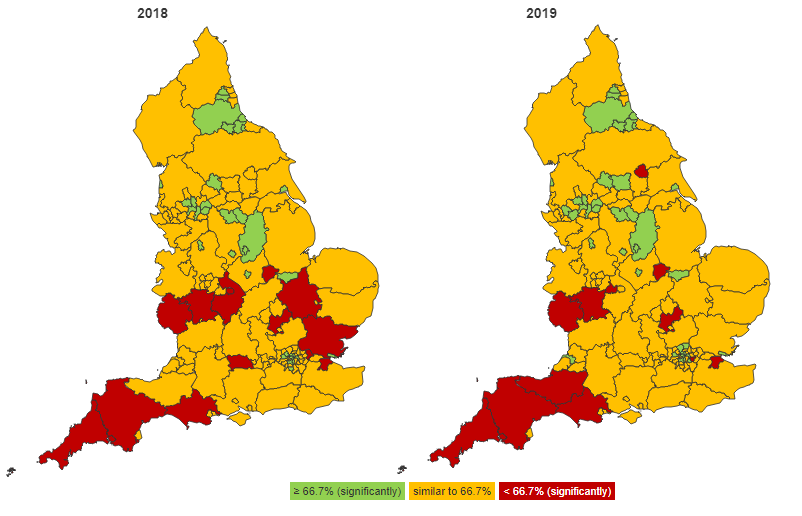
The annual EDDR has remained relatively constant over the last three years since the indicator was first introduced, with an England value of 67.5% in 2018 and a slight increase to 68.7% in 2019.
Looking at the variation between county and unitary authority areas (see maps below), 90% of areas are similar to or above target value with 25% of all areas achieving an estimated dementia diagnosis rate significantly higher than the target rate. This is an increase from 22% in 2018.
PHOF Review
In January 2019 PHE published proposals for changes to the PHOF. Indicators that were to be revised, added or removed, with a rationale for each, were outlined in our consultation. An online survey was used to gather feedback during January and February 2019.
The results were published on the 2 August 2019, available here. A full list of indicators from 2019 onwards are presented in Annex C of the document and will be implemented from November 2019.
In addition to the changes to indicators, the way that the indicators are numbered will also be changed. Each of the domains will be identified by a letter: A Overarching, B Wider determinants, C Health improvement, D Health protection and E Healthcare and premature mortality. Indicators within each of the domains will be identified by the letter for the domain followed by a number.
