Last year, our Hepatitis C in the UK report, focusing on elimination, showed the first fall in deaths from severe hep C-related liver disease in over a decade.
Our latest report suggests that this decline has been sustained for a second year, although current figures remain provisional.
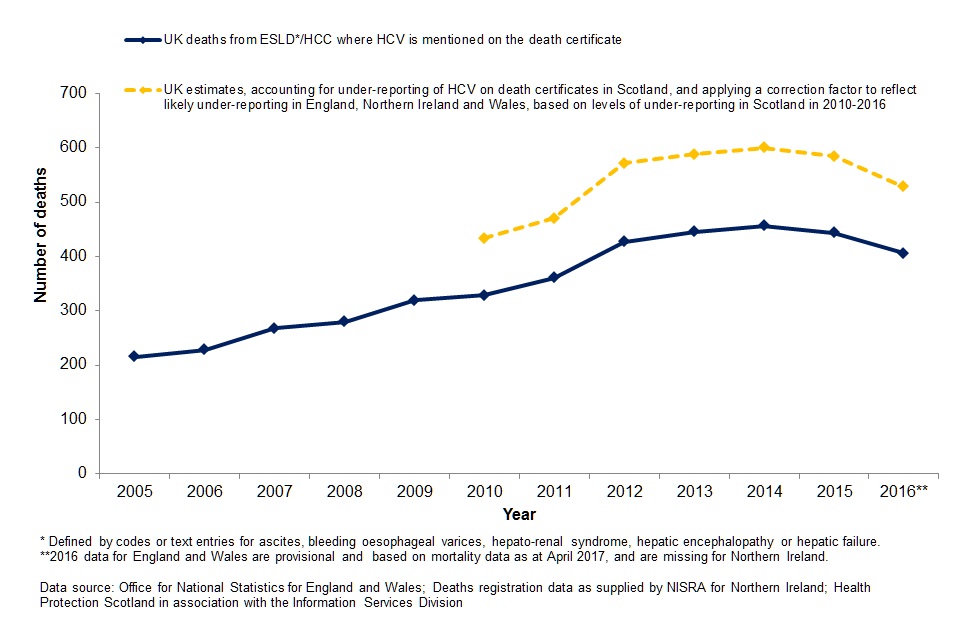 Deaths from HCV-related end-stage liver disease and hepatocellular cancer in the UK: 2005-2016
Deaths from HCV-related end-stage liver disease and hepatocellular cancer in the UK: 2005-2016
We are hopeful that increased access to improved treatments over recent years has contributed to this fall.
In previous years, people with hepatitis C faced weeks of injections and some experienced severe side-effects, meaning many struggled to complete their treatment. Now, direct acting antiviral (DAA) drugs – in tablet form – are easier to tolerate, have shorter treatment courses and have been found to be more effective in clearing the virus.
The target for NHS England is to treat 15,000 patients a year by 2020; if this can be achieved and maintained, modelling suggests this would lead to an 80% fall in severe hep C-related liver disease by 2030.
However, our ability to sustain the increase in treatment is limited by our capacity to find and treat those undiagnosed, and to help those diagnosed but untreated to engage with accessible treatment services.
Important work continues to increase testing among high risk groups, including those in prison and people who currently inject drugs.
But there are many who contracted the virus years – even decades - ago, who are not, or are no longer, in contact with services that would necessarily think to offer them a hep C test.
Where infections were acquired many years ago, disease can be more advanced, increasing the urgency for testing and prompt treatment to improve their outcomes.
Previous studies suggest over half of prevalent infection in England is among those who acquired their infection via past drug use and other routes, like blood transfusion before September 1991.
It is therefore important to raise awareness and encourage testing in these groups too.
Raising awareness among GPs is important, so they can recognise and ask about risks for infection. Free online training resources and an e-learning module are already available from the RCGP to help them do this.
Helping people to realise their own need for testing is also crucial, which is why we have worked with The Hepatitis C Trust and World Hepatitis Alliance to promote a quick online quiz.
The quiz helps to identify whether you may have been exposed to the virus and would benefit from a test. It takes less than a minute – why not try it now?
Overall, our report suggests there are challenges ahead, locally, nationally and globally. Latest WHO estimates show global deaths from viral hepatitis in 2015 are similar to those from tuberculosis (TB), and higher than those from HIV or malaria.
However, increased interventions have led to a decrease in mortality from TB, malaria and HIV over recent years, while global deaths from viral hepatitis are continuing to rise. It is encouraging that, in UK, we seem to be reversing this trend.
More still needs to be done to improve prevention, raise awareness, increase testing and get more diagnosed individuals into treatment and care, and we continue to work with our partners to meet these challenges.
This year we established a new multi-agency National Strategic Group on Viral Hepatitis (NSGVH) to bring together partner organisations to improve health services, minimise the number of new infections and reduce the health consequences of viral hepatitis for people in England.
Through effective monitoring and partnership working, we have the potential to save thousands of lives. Our progress so far is encouraging, but we must tackle the challenges ahead if we are to achieve our vision of eliminating hepatitis C as a major public health threat.
Share our quiz which helps people identify their risk of hepatitis C.

1 comment
Comment by Thelma King Thiel posted on
What is missing is any mention of promoting primary prevention by educating all children in schools about their miraculous life sustaining liver and why and how to protect it from harm. Tragically uninformed individuals are unknowingly participating daily in liver damaging activities that can lead to cirrhosis and liver cancer. . Viruses, excess in drugs, alcohol and fatty foods can kill liver cells that perform mini miracles converting the food they ingest into hundreds of life sustaining body functions 24/7.
visit liver-health.org to learn about your liver